Tailored Adherence Incentives for Childhood Asthma Medications (TAICAM): Using Incentives and Mobile Health to Improve Medication Adherence for Children with Asthma
Statement of Problem
Urban racial/ethnic minority children are disproportionality impacted by asthma and are five times more likely to die of asthma compared to their non-minority peers. While many factors contribute to these disparities, non-adherence to asthma medications is one that is well-documented and where there is potential for improvement.
Inhaled corticosteroid (ICS) medications are highly effective in improving asthma control and reducing morbidity, and can reduce the number of days when children experience symptoms, emergency department (ED) visits and hospitalizations. Yet adherence is low among certain high-risk populations. Compared to average medication adherence rates of around 50%, urban racial/ethnic minority children have average adherence rates between 11-37%.
Technology-enhanced reminder systems have shown promising results for improving medication adherence in select populations. Few studies, however, have attempted to leverage mobile health technology and incentives to improve medication adherence in children with high-risk asthma. Broader challenges also exist in engaging both caregivers and children in asthma management and ensuring sustained behavior change when incentive programs conclude.
Description
Tailored Adherence Incentives for Childhood Asthma Medications
Tailored Adherence Incentives for Childhood Asthma Medications
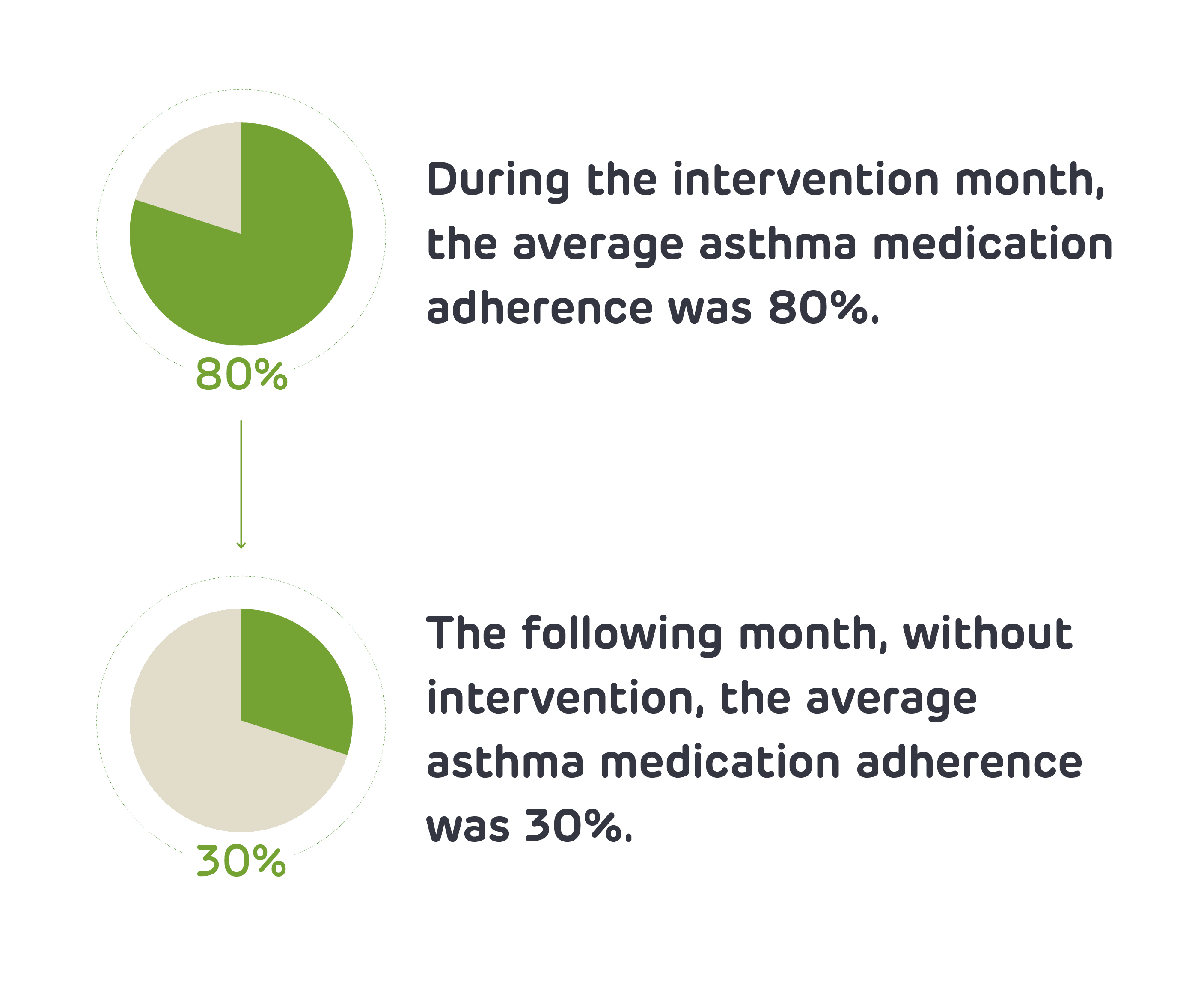
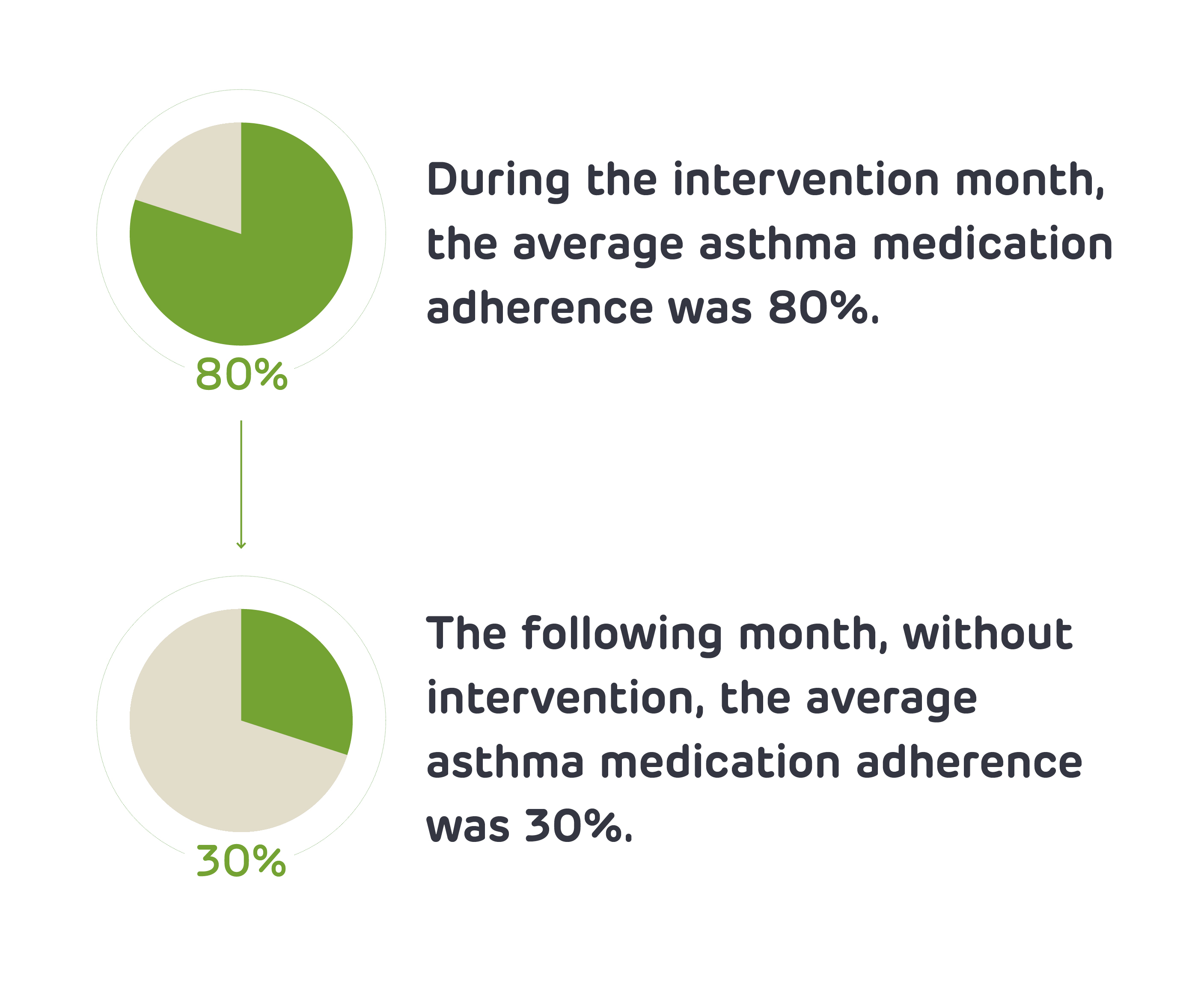
Medication adherence was near optimal in the intervention month, but dropped off when reminders and incentives stopped.
To better examine the potential of technology and incentives for families dealing with high-risk asthma, our team completed a series of studies to develop an intervention aimed at improving asthma medication adherence. After identifying important logistical  considerations and design improvements for adapting such interventions to high-risk populations in two previous studies, the latest pilot incorporated gain-framed incentives for kids, which allows them to earn a reward for performing a particular behavior. In this case, we provided children with an incentive to take their asthma medication—they could earn up to $1/day for 30 days for perfect medication adherence. We also placed an electronic sensor on the child’s asthma inhaler and downloaded a mobile app onto their caregiver’s smartphone. The app provided daily medication reminders to the family and our study team sent weekly feedback on both the child’s adherence and incentives accumulated.
considerations and design improvements for adapting such interventions to high-risk populations in two previous studies, the latest pilot incorporated gain-framed incentives for kids, which allows them to earn a reward for performing a particular behavior. In this case, we provided children with an incentive to take their asthma medication—they could earn up to $1/day for 30 days for perfect medication adherence. We also placed an electronic sensor on the child’s asthma inhaler and downloaded a mobile app onto their caregiver’s smartphone. The app provided daily medication reminders to the family and our study team sent weekly feedback on both the child’s adherence and incentives accumulated.
Of the families we approached with the most severe asthma, we enrolled nearly 70% of children with 80% follow-up, demonstrating both robust family engagement and retention. Over the course of the intervention month, families received reminders, feedback and incentives. During this time, average medication adherence was 80%. However, in the following month when families did not receive any of this support, adherence dropped to 30%. These findings demonstrate the feasibility of this pilot incentive-based intervention in engaging caregivers and children with high-risk asthma in regular medication use, and indicate there is room for improvement in medication adherence.
In the next project phase, we will continue to apply behavioral economics principles to promote medication habits during a period of childhood when many behavior patterns are established. We will conduct a randomized control trial with children ages 5-12 who take daily ICS medication and who have had at least two asthma exacerbations in the preceding year (any combination of hospitalizations, ED visits or outpatient visits where oral steroids were administered). To test the intervention with a larger number of families, we have integrated the Propeller Health inhaler sensor platform with the Way to Health behavioral incentive research platform at the University of Pennsylvania to automate the calculation of incentives and adherence feedback to participants.
Building on the pilot study, this project aims to determine if this combination of technology and incentives works to enhance ICS adherence and decrease ED, hospital, and oral steroid use in high-risk children. Additionally, we will characterize groups of high-risk children with similar patterns of ICS adherence, identify potential ways to maintain or improve adherence, and assess the acceptability of the intervention among children and caregivers. During this next phase, we will also conduct health care provider interviews to identify provider- and care network-level facilitators and barriers to integrating an incentive-based mobile health intervention in the clinical setting.
Next Steps
This approach and subsequent results will add to the evidence base on how best to engage children with high-risk asthma and their families in their asthma care and understand the waning effects of financial incentives on asthma medication adherence.
This project page was last updated in May 2021.
Suggested Citation
Children's Hospital of Philadelphia, PolicyLab. Tailored Adherence Incentives for Childhood Asthma Medications (TAICAM): Using Incentives and Mobile Health to Improve Medication Adherence for Children with Asthma [online]. Available at: http://www.policylab.chop.edu. [Accessed: plug in date accessed here].