Ensuring the Future of Health Care Coverage and Access for Children and Families
Statement of Problem
Health insurance coverage, particularly for children, is facing a time of significant transition. Numerous forces are steering public and private coverage in new directions.
While employer-sponsored insurance (ESI) was the standard-bearer for high-quality coverage for some time, working families have seen significant changes to the affordability of private health insurance coverage for their children in the past decade. Even since the advances of the Affordable Care Act (ACA), the challenges for families with commercial health insurance have only become more apparent. Premiums and deductibles for private family health insurance have nearly doubled, far outpacing the growth in median household income. Even those with insurance are arguably underinsured, meaning their insurance fails to provide them with meaningful financial protection from the costs of health care. Now, the COVID-19 pandemic and resulting financial crisis have further illuminated the need for a system that provides all children and families with continuous, comprehensive coverage not tied to employment.
In recent years, families seeking affordable, comprehensive coverage options for their children have increasingly turned to public insurance programs like Medicaid and the Children’s Health Insurance Program (CHIP), which offer low- or no-cost, comprehensive, child-specific plans. In fact, PolicyLab research published in JAMA Pediatrics in 2015 showed that children on state CHIP plans are more likely to have dental and preventive medical visits, and to have all of their medical needs met.
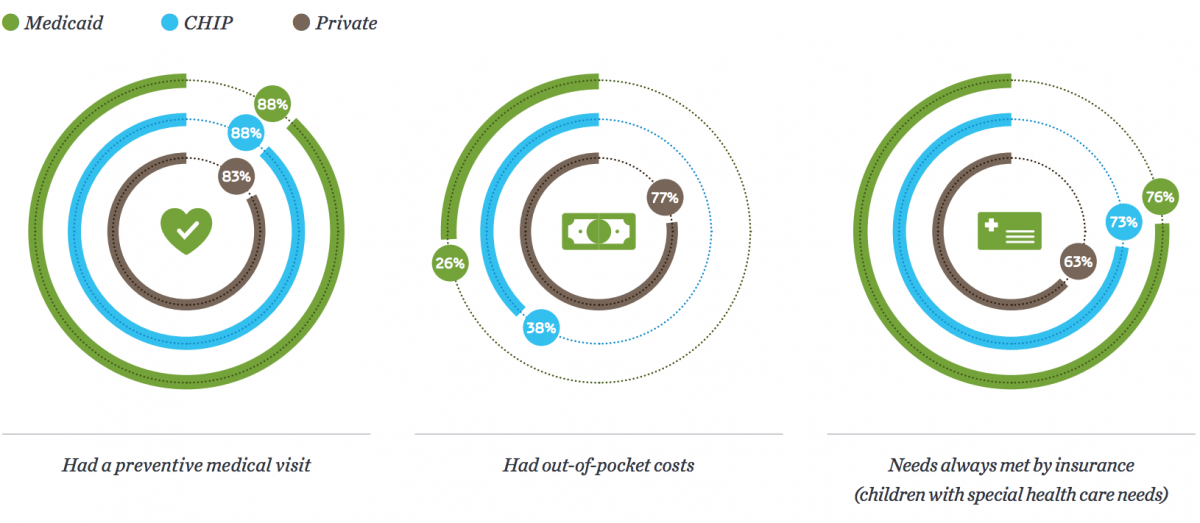
The Children's Health Insurance Program (CHIP) and Medicaid provide more affordable and comprehensive health care coverage than private, employer-sponsored coverage.
Thanks to Medicaid and CHIP, the U.S. was close to achieving universal health coverage for children—more than 95% in 2016—but unfortunately, this trajectory has been undermined in recent years.
Between 2018-2019, 320,000 children lost health insurance coverage—the largest uptick in more than a decade. These numbers reflect insurance trends pre-pandemic, and we anticipate coverage losses will continue to rise as we more fully understand the loss of ESI during the ongoing economic crisis. At the same time, enrollment in Medicaid and CHIP is on the rise, serving as an even greater safety net for families amid the pandemic. These programs, however, are under considerable strain with less funding available to meet a growing need. As states navigate an uncertain financial landscape, PolicyLab will continue to inform and advocate for policy changes that address the issue of underinsurance for those with commercial insurance and offer greater access to public insurance options for low- and middle-income families, including those who are undocumented.
Description
Health Insurance Coverage of Children In Working Families
Health Insurance Coverage of Children In Working Families
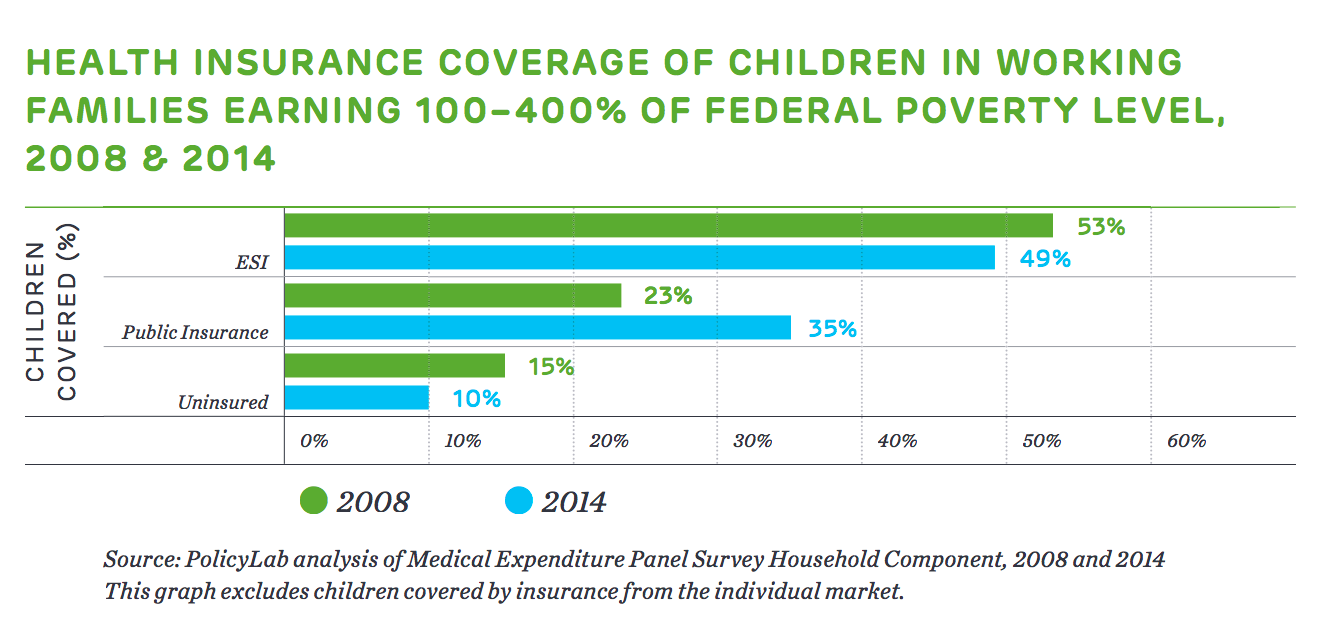

Today, more and more low- and moderate-income working families (earning 100–400 percent of the Federal Poverty Level) are shifting their children to public insurance.
Today, more and more low- and moderate-income working families (earning 100–400 percent of the Federal Poverty Level) are shifting their children to public insurance.
Our research aims to understand how both public and private insurance meet the health care needs of children and families. In 2016, PolicyLab researchers examined the coverage rates for children from low- or moderate-income households in which at least one parent had ESI from 2008-2013. We found that low- and moderate-income families increasingly moved away from covering their children through ESI. In 2013, 15.2% of children in families with incomes of 100-400% of the federal poverty level (FPL) (or $23,550-$94,200 annually for a family of four) were not covered by their parents’ ESI, but by public insurance offered through Medicaid or CHIP—an increase from 12.1% in 2008. This phenomenon of splitting insurance was greatest in families with incomes of 200-299% of FPL as, in 2013, roughly one in eight families in this income bracket insured their children through CHIP or Medicaid. Additionally, among families within this moderate-income bracket, we found an increase in uninsurance, likely due to more restrictive eligibility levels for CHIP and Medicaid in their states—early evidence of an erosion of the health coverage for children.
Following this study, we wanted to understand where parents worked and if that impacted their children’s likelihood of being covered by Medicaid and CHIP. We conducted a national study, published in Health Affairs in 2019, of working families making more than 100% of the FPL, categorizing parents by whether they worked for small or large, private companies or were employed in the public sector. Our findings showed that low-income families, with parents working at all employer types, increasingly enrolled their children in public insurance between 2008-2016. This was particularly true among low-income parents working for small businesses—public insurance coverage for kids in these families jumped from 53% in 2008 to 79% in 2016. However, our most surprising finding was that of the 8.6 million children in working families who are covered by public insurance, more than 70% have a parent who works at a large, private company. This indicates that even in sectors that have historically provided more robust health benefits to their employees, employer-sponsored dependent coverage is becoming prohibitively expensive for working families. Medicaid and CHIP, which for decades have provided a safety net for some of our nation’s most vulnerable youth, is now serving as a key structural support to millions of middle-class working families.
Next Steps
Our research illustrates a dramatic shift in the landscape of children’s health insurance coverage, with families moving their children from employer-sponsored insurance to public programs. This change is happening at a faster pace than policymakers are able to keep up, leaving many unanswered questions about the future of affordable, high-quality coverage for children. While the emergency measures taken in response to the COVID-19 pandemic have been essential for shoring up coverage for children and families during this time of crisis, they have done little to overcome fundamental issues of underinsurance faced by families.
Using PolicyLab’s menu of policy options for state and federal leaders, our research and policy teams continue to work with key stakeholders to determine crucial policy levers for increasing access to health care coverage for children and families. In future research, we will seek to better understand how families make choices in response to federal and state policies that affect the cost and comprehensiveness of health insurance coverage. As underinsurance becomes increasingly common, our research will help shed light on the types of families affected by these changes.
Based on our research, we aim to preserve Medicaid and CHIP as comprehensive programs with eligibility requirements that reflect the families depending on them for affordable, high-quality care for their children. One tangible opportunity to support this goal is the permanent funding of CHIP, the benefits of which we outlined in a 2022 Health Affairs Forefront blog post.
This project page was lasted updated in August 2022.
Suggested Citation
Children's Hospital of Philadelphia, PolicyLab. Ensuring the Future of Health Care Coverage and Access for Children and Families [Online]. Available at: http://www.policylab.chop.edu [Accessed: plug in date accessed here].