COVID-19 Outlook: Spring Planning for In-person Schooling Can Continue
Once again, in the weekly update to our COVID-Lab forecasting model, we see continued declines in COVID-19 hospitalizations and case incidence throughout the country. With each week, these improving forecasts make us optimistic that rates will continue falling well into spring. Here are some more specifics about this week’s main findings:
- Test positivity rates across the 821 counties included in our model fell to an average of 7.4% this week. This is down from 8.7% last week. More specifically, 70% of the counties we follow are now below 9% testing positivity, and 30% are below 5%.
- Nearly 70% of the counties included in our model are now seeing fewer than 200 weekly cases per 100,000 individuals. This includes some larger counties that have gone below 100 weekly cases: San Francisco, Calif. (98 per 100k); Minneapolis, Minn. (90 per 100k); St. Louis, Mo. (67 per 100k); and Honolulu, Hawaii (26 per 100k).
- We are also seeing significant declines in case incidence in the major metropolitan areas of Texas, from Dallas and Fort Worth to Houston and San Antonio. Our forecasts for these cities anticipate continued declines over the next four weeks.
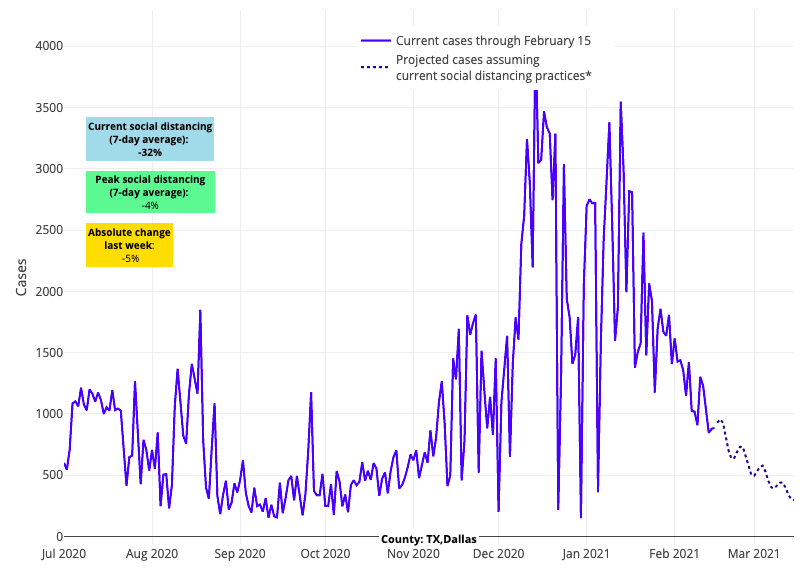
Above are the projections for Dallas County in Texas.
- National hospital census for COVID-19 has fallen to half of what it was at the beginning of 2021, with 70,000 individuals currently hospitalized. This includes a two-thirds decline in patients hospitalized for COVID-19 in California, where hospitalizations have fallen below 1,000 and deaths have dropped below 200 per day.
- Colorado is an area of some concern, as the state once again experienced increased transmission rates this past week, with Colorado Springs leading the way. Case incidence is growing in counties around Denver with reproduction numbers (a measure of transmission) exceeding 1. While this requires monitoring, current incidence and test positivity rates in this area are still better than they were in the fall.
- Counties in Tennessee also saw increased rates of transmission this past week, with Nashville reporting growing PCR testing positivity and a reproduction number that exceeds 1.
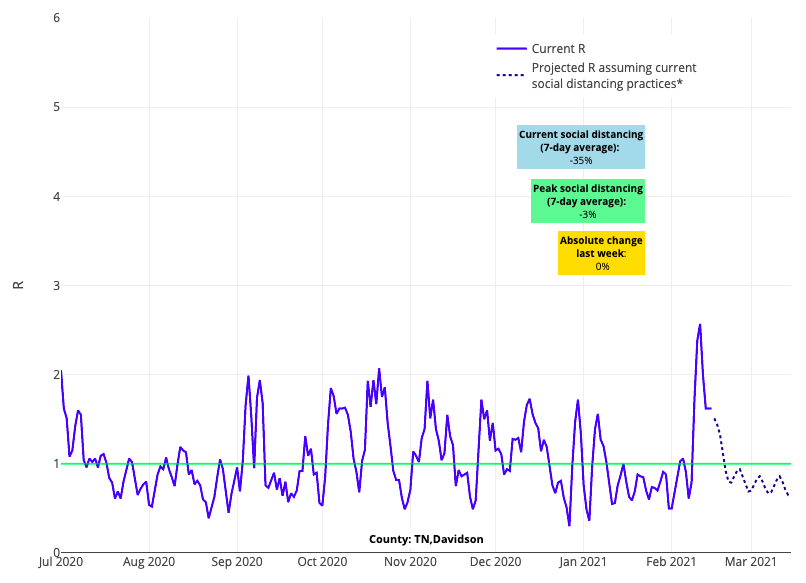
Above is the reproduction number projections graph for Davidson County (Nashville) in Tennessee.
Overall test positivity and case incidence metrics continue to be favorable. The concerns about regional resurgence risk following the Super Bowl have not materialized in New England, Tampa Bay or Kansas City. Even in Colorado and Tennessee, where increasing transmission bears close watching, the net effect continues to be declining hospitalizations and emergency department visits consistent with other areas of the country. We do continue to see lagging improvement in pediatric COVID-19 hospitalizations compared to adults. However, we were encouraged to see in this week’s data that fewer states are reporting increases in pediatric hospitalizations, and some have moved past their peaks. Finally, we are just at the beginning of another major American event, Mardi Gras. Fortunately, Louisiana’s parishes are currently seeing reproduction numbers below 1, but large gatherings have the potential to fuel transmission, so we will be monitoring for subtle increases in case incidence in the coming weeks.
Breaking Down the Criticism of the New CDC School Guidance
These developments are certainly welcomed as schools throughout our region, and elsewhere, are deliberating their ongoing reopening plans. To that end, last week, the Centers for Disease Control and Prevention (CDC) released long-anticipated updates to its school reopening guidance. Overall, the guidance reflects the evolution of a year’s worth of highly debated recommendations, distilling those that have stood the test of time and abandoning those that have failed to add value. Already, the specificity of the guidance has been met with some criticism, particularly the recommended numeric thresholds of weekly case incidence and PCR testing positivity to determine when to move from hybrid to full instruction, or when to move middle and high school students to more virtual instruction.
Our team’s view is that these thresholds, although conservative, should serve as approximate guides for schools developing or refining their spring reopening plans. Whether a school is bringing students back for the first time since March 2020, expanding the number of grades in a school or students in a classroom, or resuming some extracurricular activities, these thresholds can be helpful guardrails for school officials, but should not be interpreted as absolute requirements. We were also encouraged that the CDC positioned the value of surveillance testing of staff and students in schools as an approach that can bring and keep more children safely in the classroom, particularly in middle and high schools.
Much of the critique of the new CDC guidance surrounds the specific recommendation that full in-school instruction occur with continued masking and maintaining 6-feet distancing “to the greatest extent possible.” The guidance notes that when weekly cases are declining and approaching or below 50 weekly cases per 100,000 residents, this 6-foot requirement may be relaxed. The criticism of this guidance is based on the fact that few counties across the United States could achieve this standard during the current school year and, thus, this recommendation would serve as a continued barrier to in-person education for many schools. Our team moved away from recommending rigid threshold requirements last fall, as we saw how successful multilayered school safety plans have been at reducing the risk of COVID-19 spread in school buildings.
We are mindful that few schools could return to full in-school operations under strict adherence to 6-feet distancing, which is why many schools have operated with hybrid instruction models throughout this academic year. Therefore, the strength of the CDC’s thresholds should be viewed as more relative than absolute. The relative nature of the statement is inherent in the qualifying language used (i.e., 6-foot distancing “to the greatest extent possible”). Additionally, if schools cannot achieve 6-feet distancing, there still may be ample opportunity when repopulating schools to maximize distancing through the use of flex or outdoor space. This would be particularly important during higher-risk moments like lunchtime.
Ultimately, as they advance their in-person schooling plans, each school will need to consider its own community’s unique context and experience with its protocols to date. Some schools may be more ready than others, and, if so, can best determine their readiness for the next step.
Further Considerations for the Safe Functioning of In-person Schooling
Should we continue to see declining COVID-19 transmission, as our projections forecast, there are other important notes that can be considered alongside and in alignment with the new CDC recommendations. These include:
- While the CDC recommends focusing on county-level case incidence and test positivity rates in determining school plans, we have found county-level rates are not granular enough in some larger counties where there can be considerable variation across municipalities and school districts. For more pertinent measures of risk within large counties, we encourage school leaders to focus on municipal rates and whether there is evidence of linked in-school transmission. As transmission decreases, the capacity to conduct more complete contact tracing should return, making evidence of linked in-school transmission a more reliable measure of risk than it was during the peak periods of COVID-19 transmission this winter.
- We applaud the CDC for recognizing the value of assurance testing (which they label as screening) of staff and students. They have provided a framework and justification to continue weekly testing similar to what has been initiated in our region through Project: ACE-IT—and through testing programs that independent schools have implemented. We recognize that assurance testing is not possible in all locations and should not be perceived as necessary to consider a return to in-person education, but when possible, it can provide an additional layer of safety.
- The CDC guidelines provide an easy, intuitive method for considering participation in youth sports programs as we move into spring. The emphasis is on allowing outdoor sports participation when county-level weekly case incidence is below 100 cases per 100,000 individuals. We would add that, when possible, the addition of assurance testing in areas with higher case incidence and for high-contact sports can provide even greater flexibility in these recommendations. Testing can act as an additional layer of protection in safety plans that also include avoidance of locker rooms, strict observance to masking on benches and on sidelines, masking in indoor facilities, and masking on buses to and from games.
- The CDC guidelines do not address the unique needs of arts and theater programs, which may share similar, if not increased, risk to contact sports programs given practices are most often held indoors. Of particular concern has been transmission risk related to musical groups that include brass and wind instruments, choral and singing events and theater ensembles. As schools resume in-person practice and events, we would encourage them to maximize distancing and safety by identifying large venues in which to practice, encouraging mask wearing whenever feasible, and moving events outdoors when possible. Assurance testing that is being made available to athletes should equitably be considered for students in arts and theater programs and, likewise, other extracurricular activities in which close contact occurs.
- Planning for common spring school events—such as prom, spring musicals and graduation—is likely already occurring, but was not specifically addressed in the CDC guidance. We recognize the critical importance of these signature events in the lives of students, particularly high school students. (Our colleague, Dr. Rhonda Boyd, wrote a poignant blog post last year about how missing these major milestones can impact teen mental health.) Several school leaders we’ve talked with are prioritizing the use of outdoor space for these spring activities, and some are working with their local health departments on strategies to incorporate testing as a potential additional mitigation step to ensure the safety during these important events. We will be highlighting these recommendations in the coming weeks.
Jeffrey Gerber, MD, PhD, MSCE, is the associate director for inpatient research activities for Clinical Futures at Children’s Hospital of Philadelphia, and is a co-author of PolicyLab’s Policy Review: Evidence and Guidance for In-person Schooling during the COVID-19 Pandemic.
