COVID-19 Outlook: Transmission Accelerates as Thanksgiving Arrives
As many families in the U.S. prepare to gather for Thanksgiving, the magnitude of the geographic area experiencing COVID-19 resurgence is growing, particularly in the northern and mountainous regions of the country. Therefore, our blog post this week reviews the evolving county-level forecasts from our COVID-Lab forecasting model and provides guidance to communities and families in advance of the holiday. The team will take next week off and return the following week to update our forecasts for the remainder of the year.
Here is a summary of this week’s national data:
- The national average PCR test positivity rate across the 812 counties we continue to monitor in our models increased to 8.1% this week, up from 7.4% last week. Nearly two-thirds of counties had higher testing positivity than last week.
- The nation’s average reproduction number (a measure of transmission that estimates how many additional individuals, on average, will be infected by every positive case) rose slightly to 1.09 from 1.0 last week; the majority of counties we follow now have reproduction numbers above 1, indicating climbing case incidence.
- Average case incidence across the counties we’re monitoring reached 200 weekly cases per 100,000 residents again, with nearly two-thirds of counties surpassing the Centers for Disease Control and Prevention’s (CDC) threshold for high transmission of 100 weekly cases per 100,000 residents. We are now seeing case incidence surpass 300-400 weekly cases per 100,000 residents in the metro regions of Minneapolis, Minn., Detroit, Mich., Akron, Ohio, Pittsburgh, Pa., Buffalo, N.Y., Green Bay, Wisc., Phoenix, Ariz., Salt Lake City, Utah, and Albuquerque, N.M.
- Nationwide, the adult hospital census has remained stable, at approximately 40,000 individuals, but daily hospital admissions rose above 5,000 again this week—the first national increase since late August. Pediatric admissions and hospital census nationally are flat, with fewer than 200 admissions daily and 600 children currently hospitalized.
Here are this week’s regional data highlights:
- Much of the Upper Midwest is experiencing increases in case incidence, hospitalizations and fatalities. In Minnesota, 30% of ICU beds are occupied with COVID-19 patients. In Michigan, nearly 3,000 adults and 60 children are hospitalized, and daily fatality numbers are approaching last winter’s peak (approximately 50 per day). In Illinois, adult admissions and hospital census are up nearly 50% in the last two weeks. Chicago is nearing 150 weekly cases per 100,000 residents, with our forecasts showing additional case incidence increases over the next four weeks.
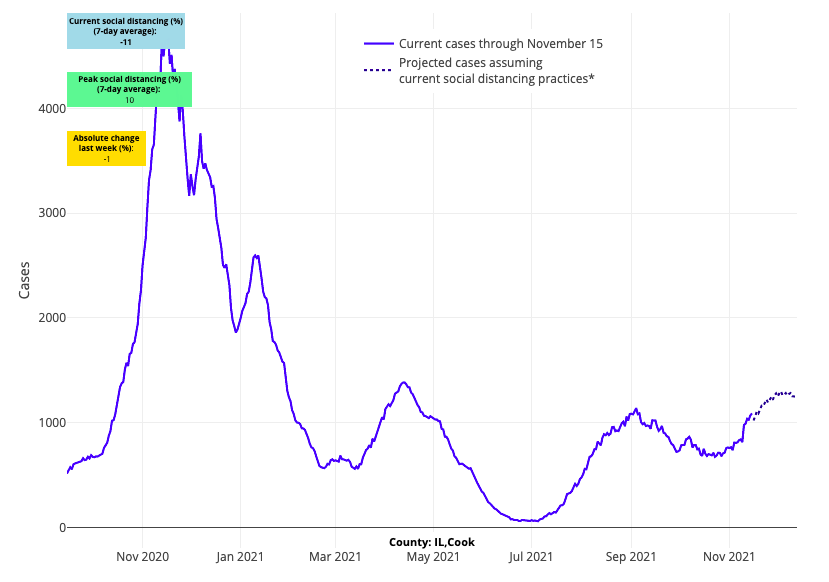
Above are the projections for Cook County (Chicago) in Illinois.
- Three of the most worrisome states in the country are Indiana, Ohio, and Pennsylvania, where we project case incidence will quickly accelerate over the coming weeks. Hospitalizations are now increasing in Indiana and Ohio, which both have below-average vaccination rates (only about 50% of residents), and Pennsylvania may be just a week or two behind.
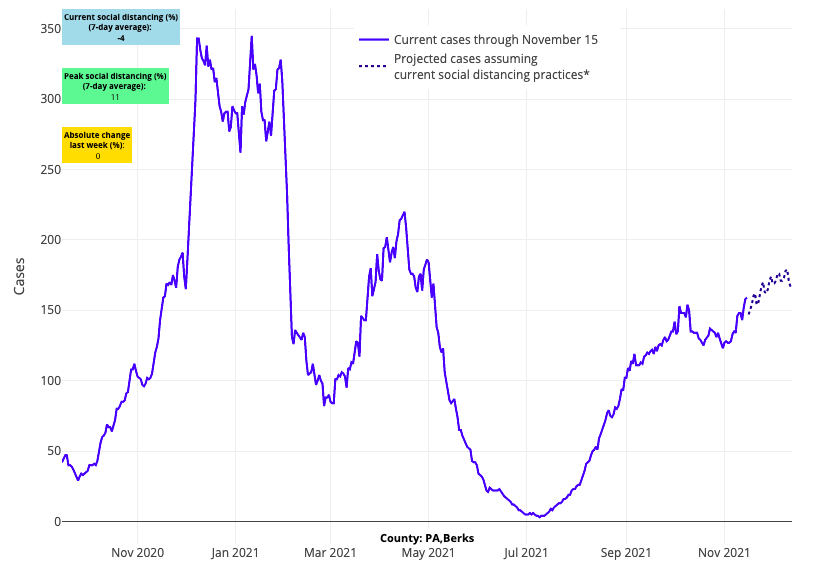
Above are the projections for Berks County in Pennsylvania.
- In the Northeast, the number of adult hospital admissions continues to grow in Maine, New Hampshire and Vermont. Of the three, Vermont, with the highest vaccination coverage in the region (72% fully vaccinated), has the lowest hospital burden (about 10 adults admitted per day and no pediatric patients hospitalized). Maine is seeing nearly 30 adults admitted to the hospital each day (census near 250), and New Hampshire is seeing nearly 40 per day (census near 300). Massachusetts continues to resist rising adult admissions, with fewer than 100 adults admitted daily across the state, but our forecasts now project increasing case incidence in Boston.
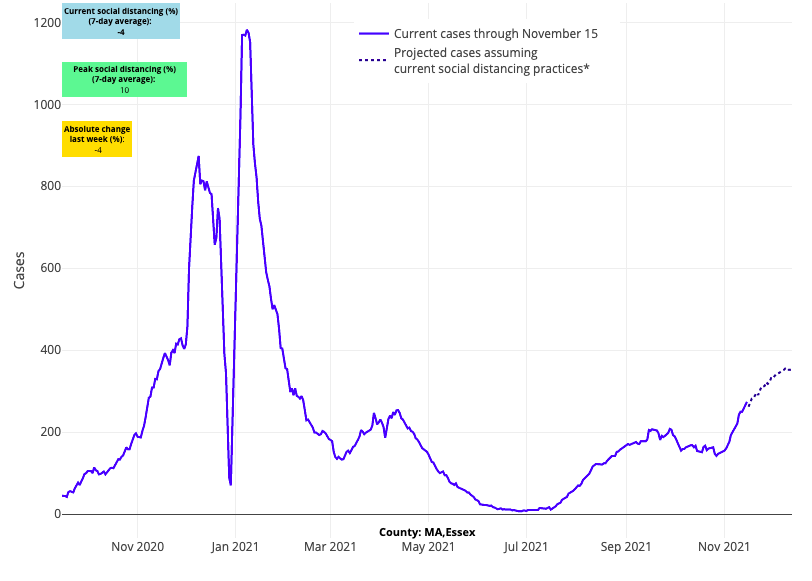
Above are the projections for Essex County in Massachusetts.
- Overall hospital admissions and census remains flat across New York state, but case incidence is again rising in the New York City metropolitan region. The city’s collar counties are likely to exceed 200 weekly cases per 100,000 residents, with the NYC boroughs not far behind.
- The lower Southeast remains stable, although further declines in transmission or hospitalizations are unlikely through the holiday season.
- While many areas of Colorado have surpassed 400 weekly cases per 100,000 residents, Denver has not eclipsed 300 weekly cases per 100,000 residents, and our forecasts project the state is moving past peak transmission. What the impact of holiday gatherings will be on the trajectory of case incidence in this region will bear watching.
- In the Southwest, Phoenix and Tucson are seeing significant resurgence, and our forecasts continue to project steep increases in case incidence over the next four weeks, which is likely to affect hospitalizations. Navajo Nation, from Arizona across into New Mexico, is seeing some of the greatest resurgence in the nation, reaching case incidence of 700-1,100 weekly cases per 100,000 residents.
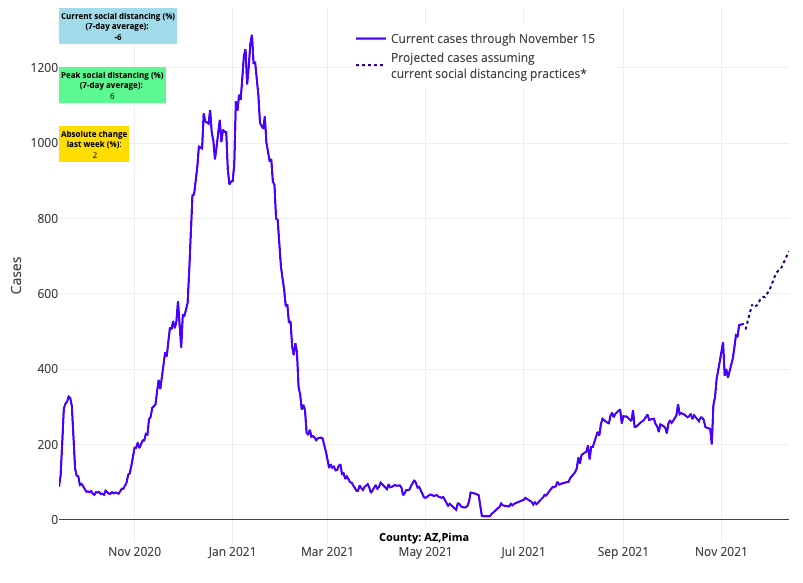
Above are the projections for Pima County in Arizona.
- Our forecasts for Los Angeles and San Francisco show flat or slight increases in case incidence over the next four weeks, even as eastern portions of California have seen growing transmission rates.
Seasonal resurgence spreads before Thanksgiving.
COVID-19 case incidence has markedly increased in multiple parts of the U.S. this week, and our forecasts now show metropolitan areas across the Midwest and Northeast will experience increasing case incidence over the next four weeks. We are monitoring hospital impacts closely, as we suspect that the magnitude of hospitalizations and fatalities we see nationally this holiday season will highly depend on how significant the resurgence is in our large metropolitan areas.
Consistently this fall, hospitalization numbers remained flat in the highly vaccinated regions of the Northeast and the West Coast despite accelerating transmission. That has begun to change, however, with increasing hospitalizations in Minnesota and Colorado, including in their more highly vaccinated city centers. In Minneapolis, where 66% of all individuals are fully vaccinated, hospitalizations have increased 20% in the past two weeks. Denver, where 69% of all adults are vaccinated, also saw a 20% increase in hospitalizations over the last two weeks. Based on these observations across the Midwest and Mountain West, large urban centers should anticipate increases in case incidence, alongside an increase in hospital admissions. The magnitude of the increase in hospitalizations will vary and likely be inversely related to vaccination rates. The current experience in Denver and Minneapolis suggests that vaccine rates in the 60% range still leave too many unvaccinated individuals vulnerable, allowing for continued increases in hospitalizations. Optimizing vaccination rates in all regions needs to remain a primary goal.
In our own state, for example, we are seeing much higher rates of hospitalizations in counties west of Philadelphia, where vaccination rates are lower and where case incidence is nearly triple that of the city. Hospitalizations had been flat or declined some from early fall but just started increasing this past week, despite more than 80% of adults in the region now being fully vaccinated. While there are reports of breakthrough severe infections among vaccinated individuals, the majority of hospital admissions are occurring among the unvaccinated.
As colder weather pushes south, the geographic areas of concern are no longer just the Upper Midwest and the Northeast. Resurgence is returning to the Heartland and Mid-Atlantic as well, which had been recovering after this summer’s wave. We’re projecting increases in case incidence in counties across Kansas, Missouri and Arkansas. Our forecasts also show rising case incidence in the Washington, D.C. area over the next four weeks.
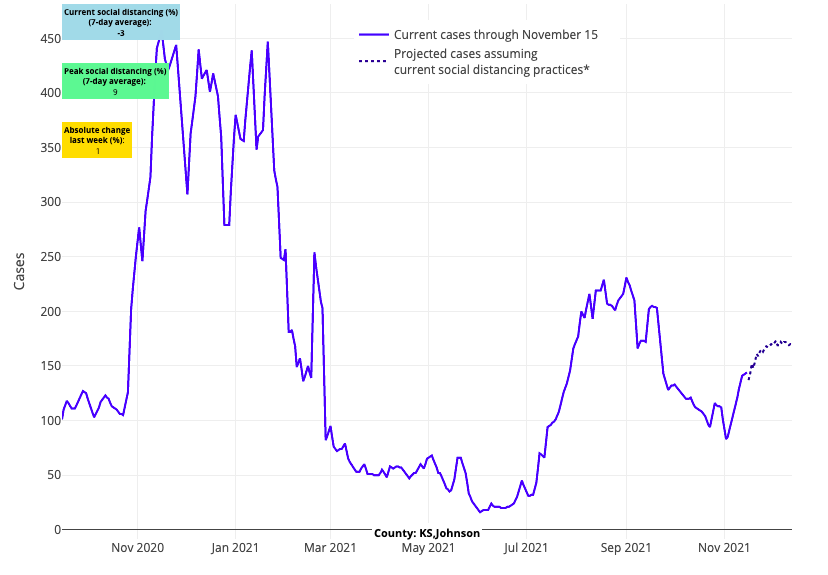
Above are the projections for Johnson County in Kansas.
All of these data lead us to believe that national case incidence will continue to rise in the coming weeks, and hospitalizations will likely follow in tandem. With that in mind, it’s crucial that we all feel prepared for Thanksgiving and the other holiday gatherings to come.
Preparing for Thanksgiving
These case incidence increases are coming at a time when many families are making plans for the Thanksgiving holiday. With pandemic fatigue omnipresent, we anticipate that numerous families will choose to resume their Thanksgiving traditions and host larger gatherings. Given where we are in the pandemic, this is entirely reasonable, but families must recognize that the risk of SARS-CoV-2 exposure remains high and, thus, holiday gatherings will still pose a risk of transmission and serious infection to loved ones during an otherwise celebratory season. While the risk will never be eliminated, there are some things that families can do to help mitigate this risk while still enjoying their holiday:
- First and foremost, take an assessment of the number of individuals that are fully vaccinated. If the entire group is vaccinated, that will be a far safer gathering. Even if a family member is not yet vaccinated, you can still encourage them to start the vaccination series now. They will not complete the series before Thanksgiving, but one dose would still be better than none.
- Families gathering with older or infirmed relatives need to recognize that even if these individuals are vaccinated, their response to the vaccinations may have been suboptimal. These families may consider pre-gathering testing to try and identify asymptomatically infected individuals. Of course, anyone with symptoms should be tested and asked to isolate. Pre-gathering testing may be especially valuable for those who live in regions with, or will be travelling through regions with, substantial case incidence.
Support of robust testing infrastructure to identify asymptomatic and symptomatic individuals will continue to be important as we navigate the coming months of this persistent pandemic. In regions with strong school-based testing programs, we recommend that schools double down on their efforts and not cut corners at the end of this year. Schools in regions with substantial community transmission might consider extra assurance testing before and after the Thanksgiving holiday. This approach can serve as an additional layer of protection to detect early outbreaks among students before classrooms empty. Identifying unexpected infections before families gather can help everyone adjust plans to protect at-risk family members throughout the holidays.
A simple illustration of the benefit of this approach comes from Project: ACE-IT, our program for school-based testing in southeastern Pennsylvania. Some schools in our region have been testing all school staff, both vaccinated and unvaccinated, throughout the fall. In the last two weeks, we detected a doubling of the infection rate. Within this group, the risk of asymptomatic infection is 70%-80% lower among vaccinated adults compared to unvaccinated adults, further confirming that unvaccinated individuals are at much greater risk for transmitting infection to others and sustaining severe infection themselves. However, it is worth noting that we are detecting some asymptomatic infections among vaccinated individuals within our testing program. When the risk of exposure rises, as is occurring in advance of the holiday season, the vaccinated may see fewer infections, but they will be of a magnitude sufficient to increase risk of transmission during holiday gatherings. So, vaccinated individuals, especially those in regions with substantial case incidence, need to be aware that it is still possible that they might transmit infections to vulnerable family members if they are not careful.
It’s fair to say that we all wished that this holiday season would be free of the need to be planful around our gatherings, but the current risk of exposure to SARS-CoV-2 remains high enough in many localities to warrant carefulness. Certainly, vaccinated individuals can take much confidence this year that the risk for severe disease for themselves or other vaccinated family members remains quite low. However, we have not yet reached a point in the pandemic where we can become complacent. Families that include vulnerable and unvaccinated people should make plans to add layers of protection to keep everyone as safe as possible when they gather together. After such a long haul, it is hard to remain patient for the brighter days ahead, but that patience may ultimately reward families from unintended consequences at this stage of the pandemic.
Our PolicyLab team wishes everyone who is celebrating a safe, healthy holiday!
