COVID-19 Outlook: Taking Stock of a Brisk Spring Resurgence
When our COVID-Lab team last checked in on April 22, we noted that some parts of the country were beginning to experience a new wave of COVID-19 infections—likely the result of increased social gatherings with reduced mask requirements. Our data reveal this surge is having a “double bump,” at least in some areas. The first bump appeared in mid-March, principally across the Northeast and Upper Midwest, and coincided with significant reductions in mask requirements. The second large bump began a week after Easter in mid-April and has continued through this week in these same regions. We have also seen areas in the Southeast, Southwest, and Pacific Northwest that were quiet in late winter very quickly enter a period of increasing COVID-19 transmission during this second period.
Our current county-level data are likely underestimating the number of new cases since many individuals use at-home testing kits, and our school-based testing data from Project: ACE-IT in the Philadelphia region support the concern for under-reporting. Project: ACE-IT data reveal that nearly 1 in 40 asymptomatic individuals in school-based settings tested weekly since the beginning of May have had detectable virus on antigen testing, up from 1 in 1,000 in early March. And yet, while it is clear that transmission has increased in this period, hospitalizations have remained quite low compared to prior waves.
The decoupling of COVID-19 transmission rates and hospitalizations that has been observed over the last year is why rates of emergency department visits and hospitalizations, not case incidence data, should serve as our guide for the true disease burden in a community. In fact, the Centers for Disease Control and Prevention (CDC) updated its guidance to rely principally on hospital impacts in determining the nature of community COVID-19 responses.
It is true that in recent weeks hospitalizations have increased again. However, as of now, the proportion of hospitalizations relative to case incidence is less than what we experienced during the winter seasons of 2020 and 2021. Hospital census nationwide is fewer than 25,000 individuals, more than 80% below where it was last winter. Additionally, the rate of growth in ICU admissions in recent weeks has been more modest than during previous surges.
There are likely multiple reasons for these epidemiological trends. First, it appears that the more transmissible omicron variants are less virulent. Second, population immunity from both vaccination and prior infection offer strong protection against severe disease. Finally, there is increasing access to effective viral therapies, which can mitigate progression from mild or moderate disease to severe disease.
At this point in time, the focus should remain on hospitalization rates. If rates remain lower than during prior surges, hospitals will be well-positioned to respond to community members in need. As we continue to remove mask requirements and return to normal activities through the remainder of spring and into summer, we should expect periods of continuing fluctuation and growing COVID-19 case incidence.
The magnitude of transmission in spring has appropriately raised concerns for the magnitude of COVID-19 transmission and subsequent hospital impacts later this fall. It is possible that a greater surge in cases at that time might lead to a more significant rise in hospital census than what we are currently witnessing. However, it is too soon to predict what the fall/winter season will bring. We will need to revisit the data as that time draws closer.
For now, we continue to encourage individuals who reside in regions with very high transmission to consider masking in crowded, indoor locations, particularly if they or their family members are at risk for severe disease. We encourage those with significant risk who have not yet obtained vaccinations or boosters to do so. Those who are sick with respiratory illness should recognize that the likelihood that they have COVID-19 is greater right now. With the degree of sustained transmission we are seeing over the month of May in the Northeast and Upper Midwest, we anticipate these regions will experience an eventual reduction in cases this summer. We are already seeing some evidence that New York, for example, may be reaching peak transmission and emergency department visits. However, we will continue to monitor these trends, particularly the emerging resurgence in areas of the Southeast, Southwest and Pacific Northwest that may extend into the summer.
Should conditions change, we’ll return with additional brief updates.
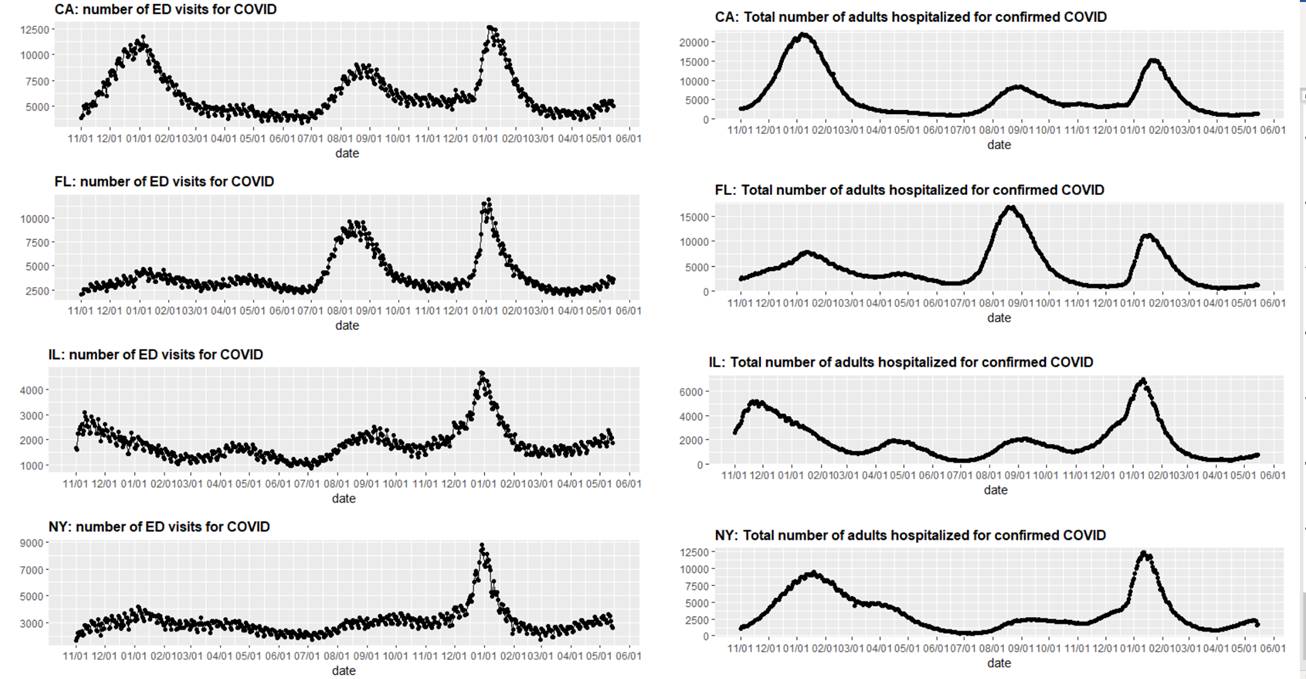
The above graphs (click to enlarge) show the number of emergency department visits and total number of adults hospitalized for confirmed COVID-19 in California, Florida, Illinois and New York.
Jeffrey Gerber, MD, PhD, is associate chief clinical research officer of Children’s Hospital of Philadelphia's Research Institute and co-author of PolicyLab's Guidance for In-person Education in K-12 Educational Settings.