COVID-19 Outlook: Looking North for Clues as Colder Weather Approaches
With another week of updated data and projections through our COVID-Lab forecasting model, here are this week’s updates:
National Assessment
- The average PCR test positivity rate across the 813 counties included in our model this week is 8.5%, down from 9.1% last week. Still, nearly one-third of counties had higher test positivity than last week. The three areas with the largest growth in test positivity include Washington, Michigan and the greater Northeast.
- Average reproduction numbers (a measure of transmission that estimates how many additional individuals, on average, will be infected by every positive case) remain at 0.85, although nearly 20% of counties continue to have reproduction numbers above 1, indicating increasing transmission.
- Average national case incidence has dropped to 220 weekly cases per 100,000 residents, with just over half of counties we’re monitoring still above 200 cases per 100,000 residents.
- Adult and pediatric hospital census remains around 50,000 and 800 this week, respectively, and is relatively unchanged compared to last week. Daily adult admissions are declining more slowly, and national pediatric admissions have plateaued at just under 200 patients per day.
Regional Assessment
- Anchorage, Alaska leads the nation in overall case incidence as it nears a weekly rate of 800 cases per 100,000 residents. We’ve observed similar case incidence across Montana and Idaho in recent weeks, and our models project sustained high case incidence for these areas in the weeks ahead.
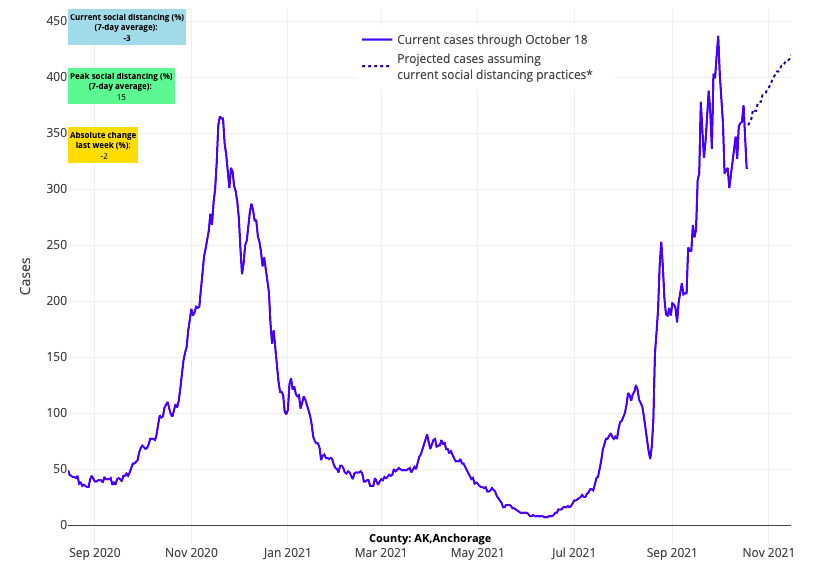
Above are the projections for Anchorage County in Alaska.
- Although Michigan’s hospitalizations continue to climb, the adult census (2,000 patients) is still only half as large as they experienced last winter. However, emergency department visits are climbing and ICU capacity has become more constrained with 25% of beds occupied by patients with COVID-19 (compared to 30% late last winter).
- Minnesota’s hospitalizations are also climbing, but like Michigan, are still at half the level of last winter. But unlike Michigan, emergency department visits are outpacing rates seen last winter, and overall hospitalizations are higher than they were during the winter surge of 2020.
- Wisconsin’s trajectory this fall has been more reassuring than Minnesota or Michigan’s. This week, falling test positivity and case incidence across a wide region of the state has our model forecasting flat, or even declining, transmission in the coming weeks.
- Overall, disease burden in the Northeast remains stable, although we are now detecting growth in areas in upstate New York, Connecticut and Massachusetts (defined by increasing test positivity and reproduction numbers); this is a significant change in the last two weeks. Vermont, New Hampshire, and Maine continue to see elevated transmission throughout this period.
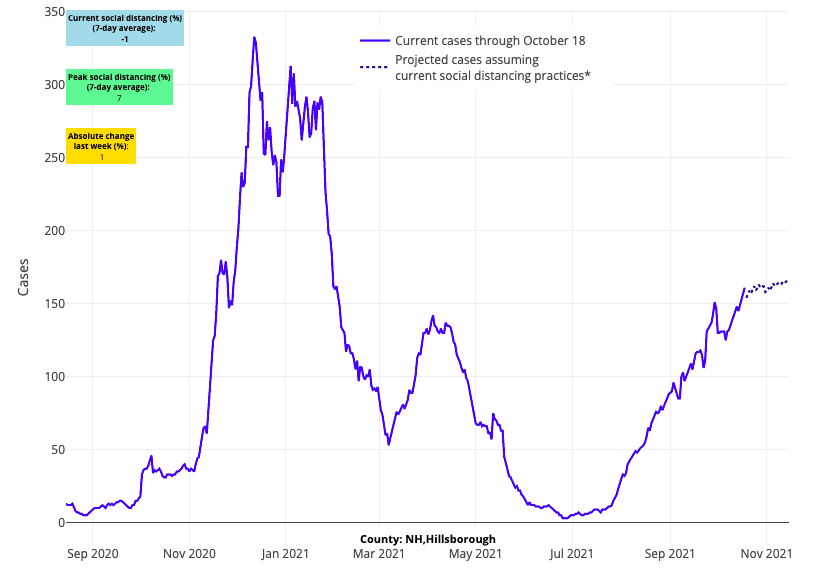
Above are the projections for Hillsborough County in New Hampshire.
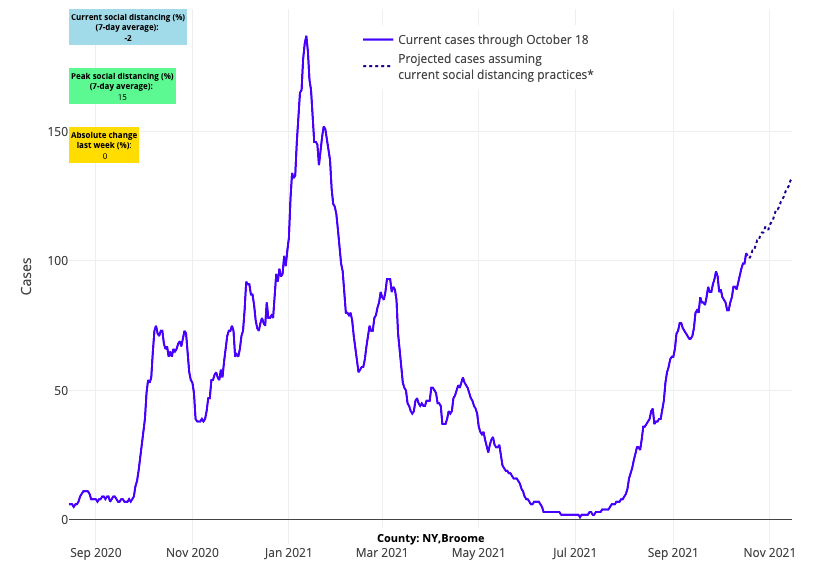
Above are the projections for Broome County in New York.
The North remains in a holding pattern as November approaches
Our team noted in our blog post last week that considerable uncertainty remains regarding the magnitude, duration and geographic footprint of COVID-19 resurgence for the winter holiday season. While a seasonal resurgence has begun in many northern areas, the impact varies, and it is likely that some locations will surge more than others.
The most important factor thus far in examining this fall’s pattern of resurgence is a region’s vaccination coverage. Substantial increases in hospitalizations across Idaho, Montana, Alaska and Michigan, for example, are easily explained by fairly low vaccination coverage in these states (ranging from 43%-58% of all residents fully vaccinated). We see encouraging signs from states and regions with higher vaccination coverage, such as Illinois, and more broadly across the Northeast, where thus far rates of full vaccination coverage range from 63% to nearly 70%. As we look at our models, we continue to be encouraged by the relatively flat forecasts in Northeast industrial cities, and in the Chicago metropolitan region in the Midwest.
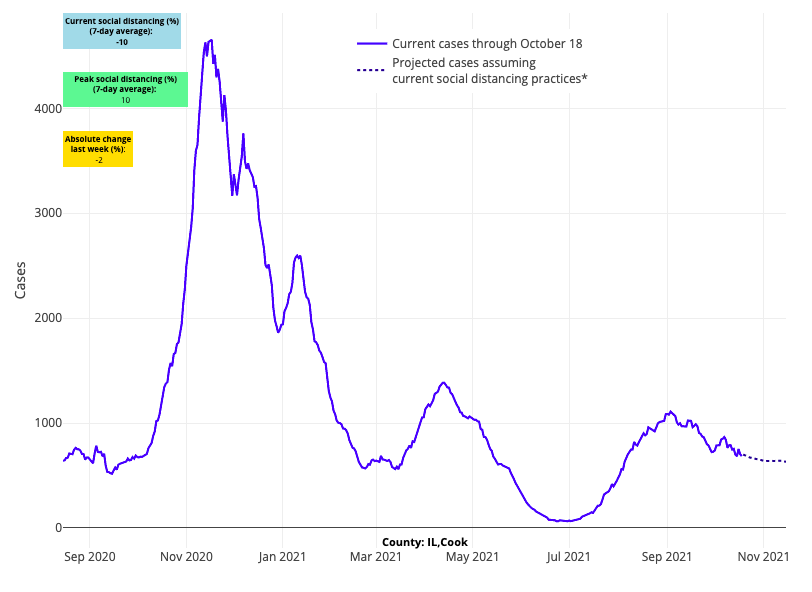
Above are the projections for Cook County (Chicago) in Illinois.
But with the coldest weather and holiday season still to come, the question becomes: will we see a surge of disease like we did last winter, or is our vaccine coverage and history of prior infection sufficient to blunt the magnitude of another winter surge? While waning immunity among adults who received the Moderna, Pfizer, or Johnson & Johnson vaccines last winter may increase the risk of transmission, booster vaccination among those eligible should help address this concern.
For guidance on what may be ahead, our team is looking north toward Canada this week where colder weather is more imminent. Of note, 73% of Canadians are fully vaccinated—a level of coverage that no state, even in the highly vaccinated Northeast, has yet achieved. And while COVID-19 infections and hospitalizations are declining throughout Canada, we see similarities with the U.S. as vaccination rates vary across provinces.
In particular, in the province of Alberta, home to Calgary, local vaccination rates are lower than Canada’s overall numbers: 66% of adults are fully vaccinated and 73% have at least one dose. These rates are comparable to those in New York and California, two more highly vaccinated states in the U.S. Alberta, however, experienced a substantial wave of resurgence in late summer and early fall, similar to the resurgence we are seeing in the Upper Midwest, though Alberta’s case growth is now abating. Moving east to Quebec province, rates of fully vaccinated individuals exceed 75% (and nearly 80% have at least one dose), and hospitalization rates are substantially lower.
Comparing Calgary or Montreal to American cities comes with some caveats. It is likely that cities throughout the U.S. have higher levels of natural immunity, given the burden of disease experienced in most metropolitan areas during prior surges. If natural immunity does help reduce disease transmission in subsequent surges, we are likely to see similar transmission and hospitalization curves in northern U.S. cities with slightly lower vaccination coverage compared to Canadian metropolitan areas. Canadian and U.S. cities also have differing rates of poverty, racial and ethnic compositions, and neighborhood crowding, and these factors can substantially alter the risk between regions.
These caveats notwithstanding, as we look to learn from Canada and to decipher the current regional variation across northern U.S. cities, we see that higher vaccination coverage will likely be necessary to avert increasing hospitalizations and deaths in many locales. It is also likely that our larger states will have pockets of increased disease activity, particularly in more rural communities, especially those where vaccine coverage is low. We have observed this trend in Pennsylvania where higher vaccination coverage in the Southeast has thus far insulated the region from rising hospitalizations that are more prevalent in other regions of the state—such as Lancaster, Pa.
Right now, America’s northern locations hang in the balance with continued uncertainty for the weeks ahead. Communities enter the holiday season with higher rates of hospitalization and transmission than last year at this time, but may benefit from the protection of vaccinations and immunity from natural infection for many individuals to help defend against severe disease in the weeks ahead. While the flatter trajectories we are observing in many cities likely suggest a winter with far fewer hospitalizations than last year, we are not yet ready to declare the worst days behind us for some regions in the north.
This is a time to remain vigilant as transmission rates rise in certain regions, and to not take for granted the proven mitigation strategies we have at our disposal, like masking in indoor public settings, promoting vaccination of adults and children alike, and adjusting our individual routines when periods of substantial transmission are moving through our communities.
