COVID-19 Outlook: The Uncertainty of What is to Come

With COVID-19 cases increasing across the country again, the importance of following local data is now more critical than ever. In parts of the South, this increase has been more rapid, resulting in a public health emergency. Other areas have experienced more modest increases in cases thus far. This week, we are providing a brief update on the data from our COVID-Lab models, which we use to continue monitoring transmission across 821 counties in the United States. We will return in two weeks with a full modeling update, including county-level case incidence projections, in anticipation of Labor Day and the resumption of more K-12 schools.
Here are this week’s updates:
- The PCR testing positivity rate increased this week in most parts of the country; the mean PCR positivity rate across the 821 counties we track surpassed 10%. Weekly case incidence is now above 100 cases per 100,000 individuals for the majority of these counties.
- Increases in case incidence are most pronounced across the Southeast. A number of counties in Louisiana, Mississippi and Florida are exceeding 400 weekly cases per 100,000 individuals. In Louisiana, some counties are seeing 1,000 weekly cases per 100,000 individuals—a number that more than doubled in the last two weeks.
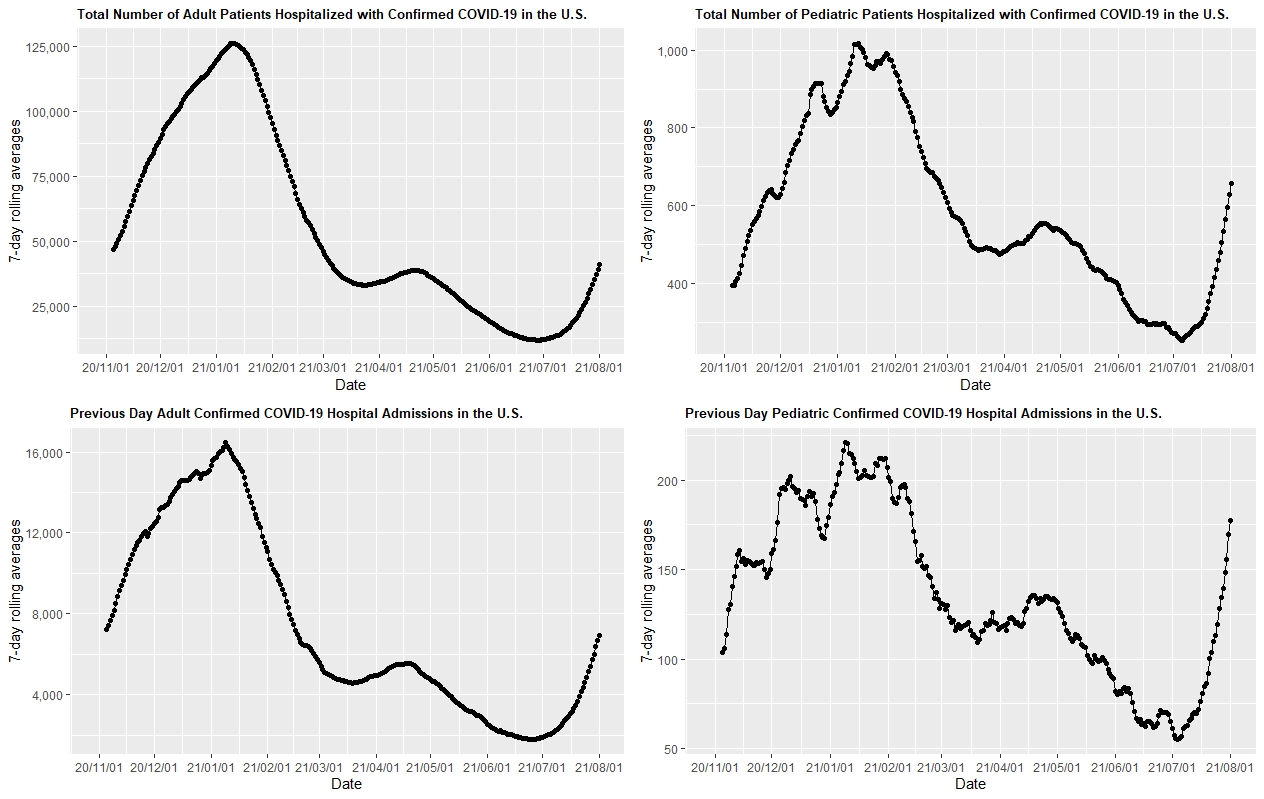
- Daily COVID-19 hospitalizations nationwide are also up to nearly 50,000 adults and 700 children. States across the South currently account for two-thirds of all hospitalizations. Louisiana has experienced a 10-fold increase in adult and pediatric hospitalizations, with U.S. Department of Health and Human Services (HHS) Protect data reporting a hospital census of nearly 2,000 adults and 40 children this week.
Total number of adult and pediatric patients hospitalized with confirmed COVID-19 in the U.S. & previous day adult and pediatric confirmed COVID-19 hospital admissions in the U.S. (click to enlarge image)
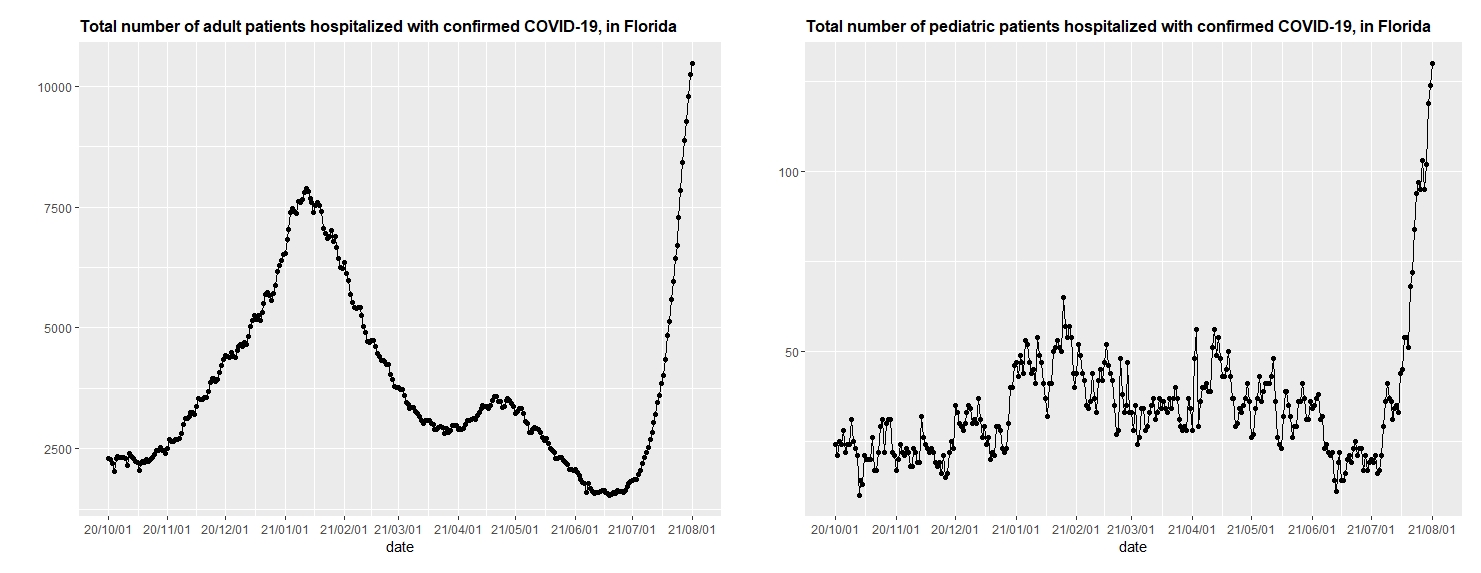
- Parts of Florida are in crisis—the state currently has 10,000 hospitalized adults (20% of the nation’s total) and 150 hospitalized children (20% of the nation’s total). Florida is again recording over 100 deaths daily.
Total number of adult patients and pediatric patients hospitalized with confirmed COVID-19 in Florida (click to enlarge image)
- Rapid growth in cases and hospitalizations is evident this week up the I-95 corridor into the Carolinas.
- Hospitalizations have quadrupled in Texas, both for adults and children. Importantly, 30% of Texas’ adult ICU beds are currently occupied by COVID-19 patients, reminiscent of past waves when hospital capacity was overstretched. Impacts are greater in southern metropolitan areas of Texas, including San Antonio and Houston, but also extend to Galveston County, which is seeing more than 400 weekly cases per 100,000 individuals.
- Growth in other locations is less rapid but bears close monitoring. In the Denver region, emergency department visits have been rising. Arizona’s COVID-19 hospitalizations have doubled to nearly 1,000 individuals in the last few weeks, which is still far off from their winter peaks of more than 4,000 individuals and doesn’t include many children. Transmission in Washington and Oregon is greater than what they saw in the spring, but for now, Seattle’s case incidence and hospitalization numbers are rising more slowly than the rest of the region.
- Even as case incidence slowly climbs in the Northeast, emergency department visits and hospitalization rates have lagged behind and showed some stabilization this past week.
Learning from Past Waves
The overall pattern of this summer’s COVID-19 resurgence mirrors that of last summer: case incidence and hospitalizations rising most dramatically in the South during times of extreme heat and humidity.
Although some of the current wave’s rapid growth can be attributed to the increased transmissibility of the delta variant, the impact of our collective behavioral changes cannot be overstated. The country is now fully open, large, unmasked gatherings are becoming common and social distancing is a thing of the past. The combination of a more easily transmissible virus, limited personal mitigation measures, and still substantial numbers of unvaccinated individuals has fueled this resurgence. Vaccinated individuals now find themselves increasingly exposed amidst growing incidence rates. This has led to some vaccinated individuals getting infected, events that have been highly publicized, including last week’s report of an outbreak in Provincetown, Mass.
While some have pointed to these reports and questioned the effectiveness of the vaccines, we see them as reassuring that the vaccines are highly effective. It’s important to remember that the vaccine clinical trials were done during a period when social distancing and mask use were still the norm. Still, as these mitigation strategies are less common in many locations, vaccinated individuals, for the most part, have been protected against severe disease and hospitalization. We are hopeful that many unvaccinated individuals are also recognizing this benefit.
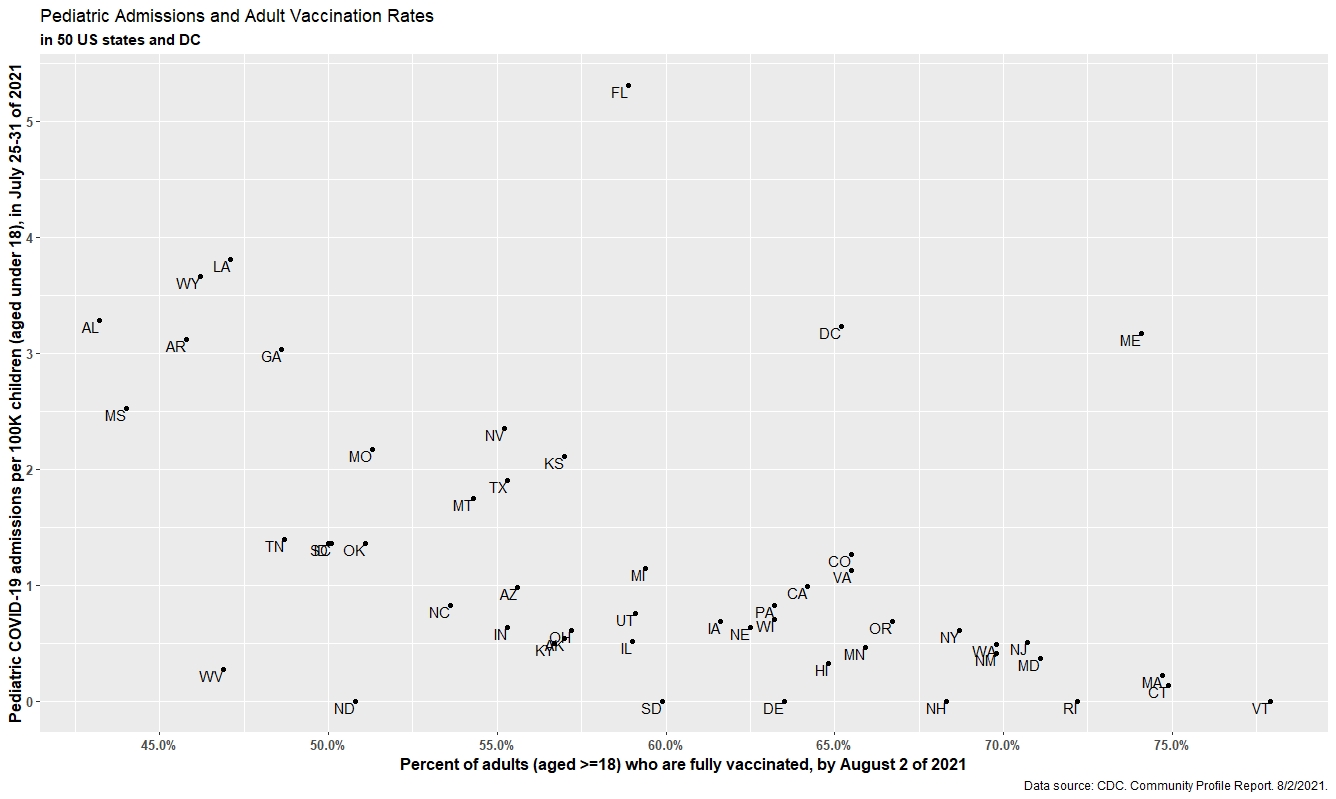
Pediatric admissions and adult vaccination rates in 50 U.S. states and D.C. (click to enlarge image)
The direction this current surge takes over the next few weeks is likely to follow similar patterns from last summer. However, the height to which this surge reaches in each location, and the magnitude of hospitalizations and subsequent deaths, will likely depend on local vaccination coverage and the willingness to utilize mitigation strategies (masking indoors or reducing gathering sizes) in areas with the largest outbreaks and surges in hospitalizations. We are happy to note that vaccinations are again on the rise, and it’s likely that employer mandates will help nudge these rates further upward. Together, optimizing vaccinations and resuming some time-limited mitigation strategies can help quell this surge.
Optimizing Vaccinations as We Prepare for Fall
Even as we take stock of a serious resurgence this summer, we must be aware of vulnerabilities that may still arise later this fall, as colder weather may pose significant risk for areas farther north. We would expect that cases in the South will begin abating in the coming weeks, but new areas of concern are likely to move northward, beginning in the Carolinas, Georgia, and Tennessee, where we’re already seeing growing case incidence and hospitalizations. The figurative “sea levels” are already rising in the Upper Midwest and across the upper Mountain States, much like they did last summer before a large outbreak occurred across the Upper Midwest. The highest transmission rates this week were concentrated in Wisconsin and Minnesota, even if these states’ overall community incidence rates are still less than those in the South. Lower vaccination rates in those locations make them vulnerable to a substantial recurrence, particularly in large cities. We need to vaccinate as many individuals as possible before fall arrives.
While we closely watch the evolution of this current surge, we remain optimistic that not all areas will see the same impact. Areas with higher vaccination rates, such as the Northeast, are likely to be more resilient in the coming months. Areas with less population immunity will likely endure higher incidence rates. We would, therefore, expect that local experience in the fall, when all schools are back in session, will be highly variable from region to region. The Centers for Disease Control and Prevention (CDC) and the American Academy of Pediatrics (AAP) have updated their guidance for K-12 schools to require masking in all locations this fall. Our school guidance provides flexibility to alter routines based on community transmission and local vaccination rates given the variability we expect to see between regions, and even schools.
We’ll be back in two weeks with a modeling update that includes case incidence projections beyond Labor Day Weekend. Stay safe out there and stay practical; if you are in a region with significant transmission, wearing your mask and practicing some more social distancing can be a short-term antidote to reaching the other side of this surge safely.