COVID-19 Outlook: Finding a New Equilibrium as We Flatten the Curve
As we analyze the second of our weekly updates to the PolicyLab COVID-Lab model, we can see that community norms and distancing behaviors are changing quickly out there. Counties continue to open at different speeds and, we assume, with varying levels of vigilance to masking and hygiene routines that can mitigate new COVID-19 transmission as people start to mix more often.
Within our team, we continue to work diligently to improve the predictive capability of our models, as well as to incorporate new information on commuting risk to better illustrate transmission dynamics across neighboring communities.
Last week, we foresaw that many areas of the south were demonstrating heightened risk for virus resurgence as they reopened compared to other areas of the country. We also kept a close eye on ongoing epidemics in the Washington, D.C. metro area and the upper Midwest. Individual counties, sometimes defined by a meatpacking facility, were also continuing to flare up in central and mid-Atlantic areas, risking spread to neighboring communities.
The news is mixed again this week, although a bit more optimistic. Areas of the south, particularly in Texas and Florida, continue to reveal some increased risk, but no worse than our predictions last week. Other counties are still seeing elevated cases, but appear to be achieving some equilibrium as their predicted case numbers are stabilizing, albeit at higher counts than they were a few weeks ago. This suggests that reopenings are affecting the ability of these communities to degrade new cases, but virus transmission is also not projected to surge. For some counties, this could also be a result of a local outbreak in a nursing home, prison, or other congregate living facility that is being contained with widespread testing and quarantine, a level of detail our models cannot detect.
For communities that have seemingly reached this equilibrium—like Atlanta, Nashville, Palm Beach, Miami, Los Angeles, and Salt Lake City—higher but flattened levels of transmission may represent the tradeoff of reopening economies, i.e. our new normal. Those areas that are more cautious with maintained distancing practices and preventing unnecessary crowding may be able to level out at lower rates. We see evidence for that in Madison, Denver and Seattle. But for those communities that choose to reopen even with higher daily circulating cases, they need to be even more careful of protecting and surveying their locations at highest risk for local outbreaks, like nursing homes and factories. Community spread in those areas could ignite easier.
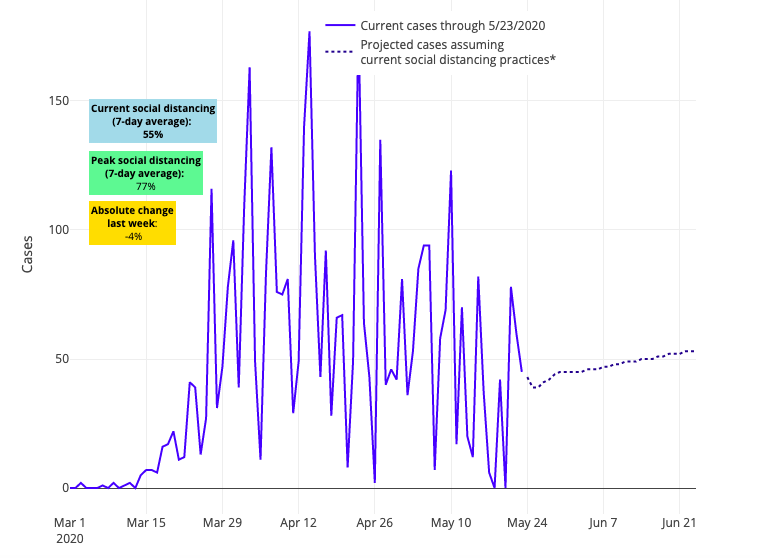
Above are the projections for Fulton County in Georgia.
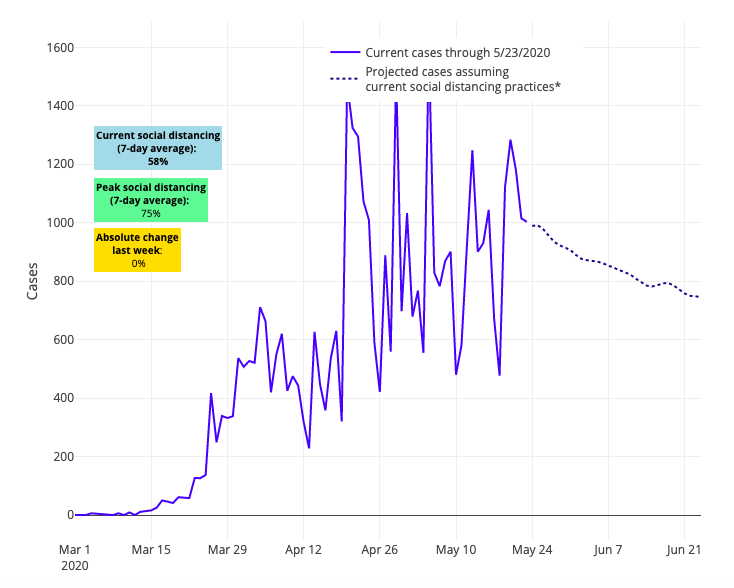
Above are the projections for Los Angeles County in California.
We will, therefore, need to carefully watch in the coming weeks the counties we’ve seen building this sort of equilibrium. To the degree that hospitalizations are not rising in a way that threatens capacity within local areas, this could be a sign that while individuals need to remain vigilant with masking and other hygiene and disinfection recommendations, those counties might not see extensive community spread. However, hospital capacity was already an issue in many rural counties before the pandemic. That makes us concerned about the rising case counts we’re projecting in Mississippi, Alabama, North Carolina, Iowa, South Dakota and Omaha, Neb. But if areas in Virginia, D.C., Maryland, or Southeast Florida can tolerate the new equilibrium without stressing local resources, they may be able to teeter in a delicate balance.
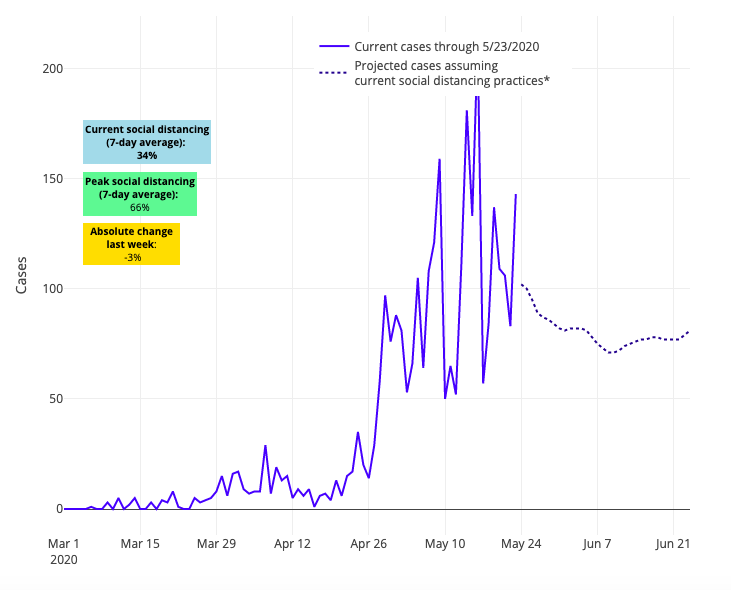
Above are the projections for Douglas County in Nebraska.
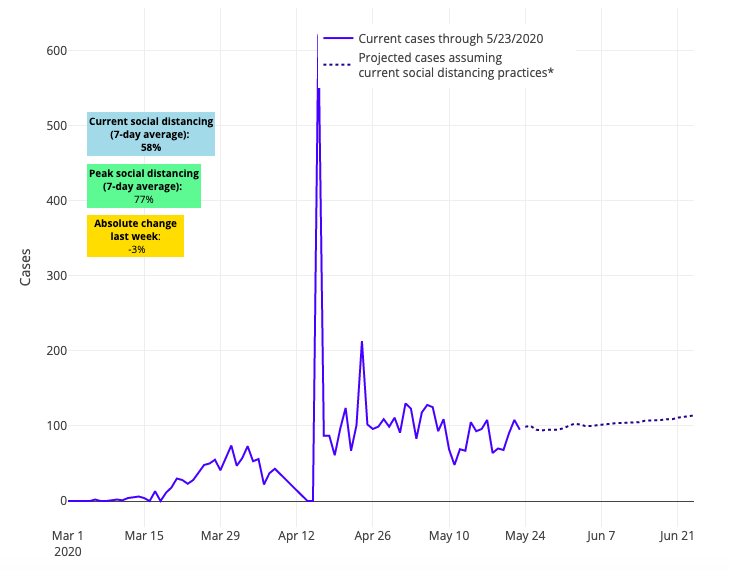
Above are the projections for Denver County in Colorado.
For those communities that are still in the midst of the epidemic, like Chicago and Minneapolis, this issue is more acute as they are still surging and will likely take weeks to stabilize with reduced stress on their health care systems.
All of this makes the next few weeks a critical time to follow the PolicyLab models. To what degree will this equilibrium hold in many places? How will Memorial Day, with its associated gatherings and travels, create a new dynamic in resurgence risk? And finally, as we reach those extreme summer temperatures and humidity levels, how will swift reopenings in many southern communities collide with the mitigating effects of hot, humid weather to affect future transmission risk? We’ll be evaluating all of this and more as we continue our weekly updates.
Our forecasts are best viewed as snapshots across time that communities can consider alongside pressure on local hospital emergency departments and disease outbreaks in neighboring areas. To the degree that all signals are detecting risk, resurgence will be confirmed. To the degree that we foresee risk that other indicators have not confirmed, we would suggest individuals adjust their routines so they can more easily adapt to periods of heightened risk—this means embracing those inconveniences of wearing masks in crowded indoor locations and washing your hands every time you enter your home. Think of our models as a dynamic early warning system that is complementary to what you are seeing on the ground in your communities, and stay tuned for more updates next week.
Gregory Tasian, MD, MSc, MSCE, is an associate professor of urology and epidemiology and a senior scholar in the Center for Clinical Epidemiology and Biostatistics at the University of Pennsylvania Perelman School of Medicine. He is also an attending pediatric urologist in the Division of Urology at Children's Hospital of Philadelphia.
