Counties are Relaxing Social Distancing. What Could That Mean in the Short-term?

It’s been two weeks since you last heard from our team at PolicyLab and the University of Pennsylvania on our county-level projections for the COVID-19 epidemic. Since then, our team hunkered down to begin incorporating the changes communities were experiencing as many people emerged from confinement during the shelter-in-place phase of this pandemic. Prompted by interest from across the country, we also focused on expanding the number of counties included in our analysis.
So, what has changed? Previously, we provided COVID-19 case projections through the summer for 211 counties with active outbreaks since early March. We drew these from a larger set of 260 counties that had cities with more than 100,000 people or were capitals within their states. As the epidemic has unfolded, many other large counties have seen outbreaks. As such, we have now expanded our models to include nearly 400 counties nationwide. These 389 counties with active outbreaks are a subset of nearly 600 counties we’re following that are home to more than 100,000 people (and not simply with a large city). They represent 68% of the population and contain 87% of all cases nationwide to date.
Apart from more than doubling the number of counties we are now modeling, we are also pivoting our strategy to shortened forecasts over a four-week horizon. And with good reason. Many counties are now reopening; people are beginning to return to non-essential businesses and other aspects of their daily lives. Long-range scenario planning worked well for supporting policymakers in the decision of when to reopen while, on average, people across the country had reduced their visits to non-essential businesses like hair salons and restaurants by 70%. When looking across our data, the conclusion we reached was that reopening was possible, but only if done cautiously and slowly. We also foresaw in our models that counties would be aided in reopening by warming spring temperatures and increasing humidity, which seem to be reducing virus transmission.
But the key now is understanding the resurgence risk as social distancing begins to change. In that light, the travel we have witnessed through our tracking of Unacast cell phone data to non-essential businesses in the last two weeks has been revealing. The lowest amount of social distancing we observed still remained about 50% as of last week in our large cities, which equates to going back about one-fourth of the way to normal travel to non-essential businesses.
However, we’re also seeing in our models that some areas—particularly in the south—that have moved more quickly to reopen are showing a higher risk for resurgence. If people in Houston and Palm Beach, Fla., for example, aren’t being cautious with masking in indoor crowded locations and with hygiene and disinfection, local governments may need to intervene again should they lose control of the epidemic.
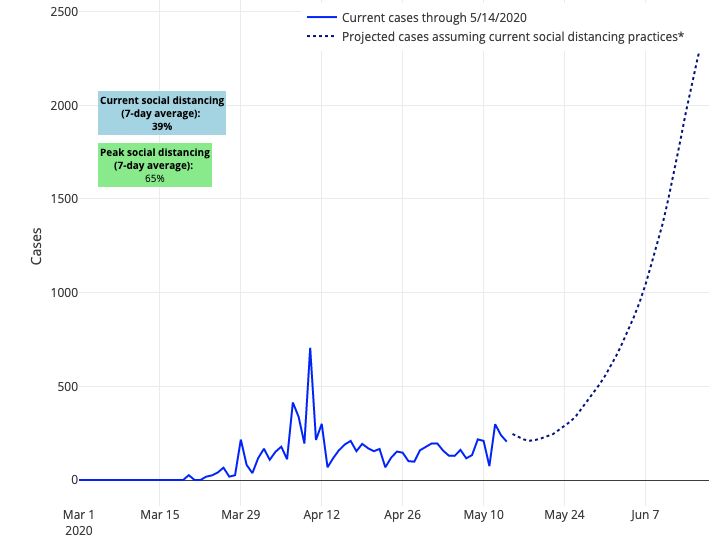
Above are the projections for Harris County in Texas.
There is also some bright news in our updated models for those communities that are remaining more cautious, or reopening slowly. Even as many in the media try to paint reopening as a binary decision—the state has reopened or it hasn’t—the truth is much more nuanced. Several governors are selectively opening regions with lower circulating cases and transmission. And when they do, most are still being cautious, reopening restaurants with reduced occupancy in many places and maintaining restrictions on large gatherings. In our data, this appears to manage the crisis well—we see evidence of this throughout Colorado, for example.
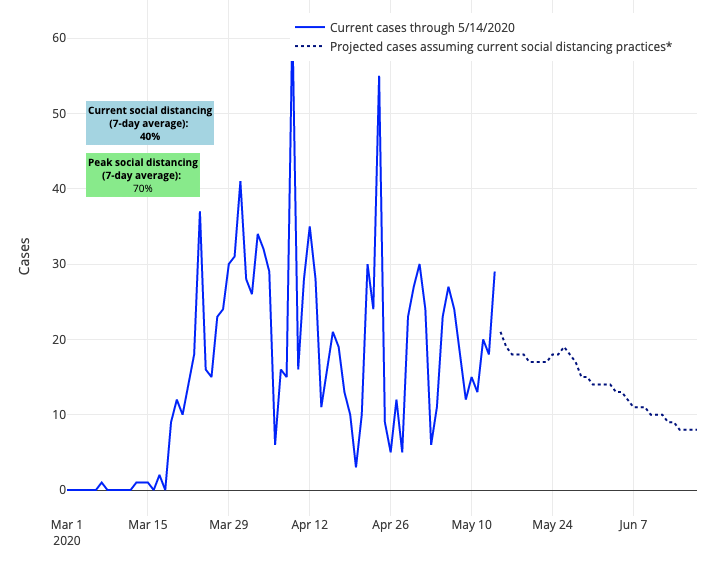
Above are the projections for El Paso County in Colorado.
Given these cautious actions by our governments, we have already seen that the predicted resurgence has not occurred in most places that are beginning to reopen—rather, daily cases are either plateauing or falling. But the picture our models are painting for Texas and Florida provide ample evidence to others who would choose to move too quickly. We see these concerns even as we adjust for additional testing capacity that might have inflated our forecasts.
As people consider our new forecasts, we would remind them that our models also foresee more heightened risk than other models for the fall, when colder, drier temperatures return. As German Chancellor Angela Merkel stated recently, “let us not squander all we have achieved.” Our goal for the summer should still be to reopen communities, but stay ever vigilant with our masking routines in indoor locations and with hand hygiene and disinfection. We should also prioritize setting up the surveillance systems our communities need to test frequently within high-risk settings like nursing homes so that we can identify outbreaks early and initiate the necessary contact tracing to effectively quarantine exposed workers and their contacts.
Our main message remains: If we stay vigilant, we can control the transmission of this virus.
Feel free to reach out to us about our new models, and stay tuned in the coming weeks for increasing sophistication of the models as we consider more complex factors that are changing, such as commuting and adoption of masking, and travel risk to areas. We intend to update our projections frequently, and hope they can be helpful to leaders as they consider how best to navigate the changes and risks in their local communities.
Gregory Tasian, MD, MSc, MSCE, is an associate professor of urology and epidemiology and a senior scholar in the Center for Clinical Epidemiology and Biostatistics at the University of Pennsylvania Perelman School of Medicine. He is also an attending pediatric urologist in the Division of Urology at Children's Hospital of Philadelphia.
