COVID-19 Outlook: Cautious Notes of Optimism During a Spring Resurgence

Below is the national outlook from the weekly update to our county-level COVID-Lab forecasting model:
- The average PCR testing positivity rate across the 821 counties included in our model is 5.8%; this is similar to the 5.7% average positivity rate from the week before.
- Nine states experienced an absolute increase of 1% or more in test positivity rates over the last week: Alaska, Michigan, North Dakota, Oregon, Pennsylvania, South Dakota, Washington, West Virginia and Wyoming. Michigan had the highest absolute increase in test positivity, going from 8% to 12%.
- The average reproduction number (a measure of transmission that indicates how many additional individuals could be infected by every positive case) across all of the counties in our model increased to 1.14, after having hovered near 1 for several weeks. Counties with reproductions numbers exceeding 1 are concentrated in the northern half of the country.
- Twenty percent of the 821 counties we follow now have 7-day average reproduction numbers above 1.25, indicating increasing transmission.
- Despite increasing test positivity rates and reproduction numbers, the nation’s hospital census remains flat at nearly 40,000 individuals. States that have experienced increases in hospitalizations over the past two weeks include Connecticut, Delaware, Maryland, Michigan and New Jersey.
Specific areas we are monitoring closely:
- Metropolitan regions with reproduction numbers above 1.25, indicating substantial transmission, include Detroit and Macomb County, Michigan (1.5), Chicago (1.43), Baltimore (1.42), the Philadelphia area (1.36-1.5) and Minneapolis (1.32).
- Again this week, Michigan saw increases in test positivity rates, emergency department visits and hospitalizations (including an ICU capacity that quickly rose to 25%). However, there are signs from the past few days that the state’s metropolitan areas may be reaching a peak for this most recent surge, including a plateau in reproduction numbers and a slowing rate of growth in emergency department visits and new hospitalizations.
- In the Chicago region, test positivity and case incidence increases are following a similar trajectory to that experienced by Detroit just a few weeks ago. Hospitalizations are also growing now throughout Illinois, albeit at lower rates than during the fall.
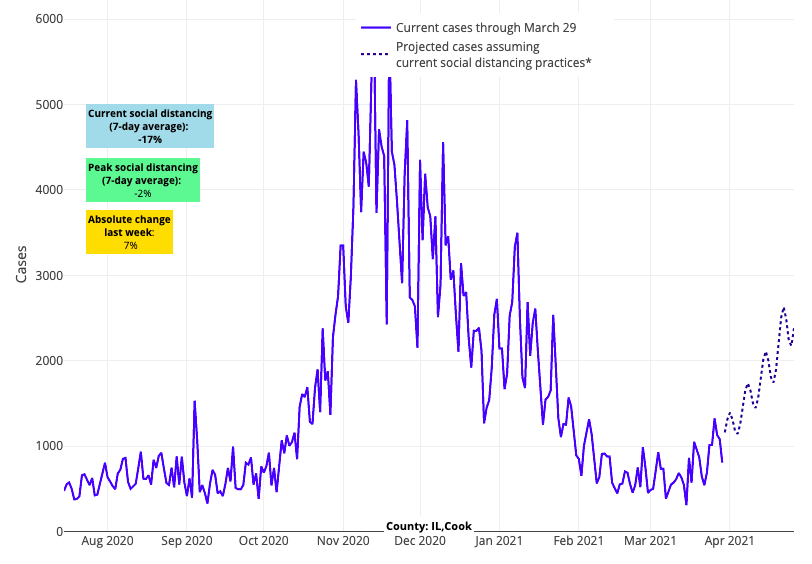
Above are the projections for Cook County (Chicago) in Illinois.
- In Boston, reproduction numbers and case incidence are increasing at steady rates. Hospitalizations and deaths are beginning to rise again, although the region has not seen the acceleration of test positivity recently experienced by Michigan and Illinois. Neighboring states of Maine, New Hampshire and Rhode Island are fortunately showing stable transmission and hospitalizations. Connecticut, however, also experienced a rapid acceleration in hospitalizations this week.
- The New York City area is showing signs of stabilization this week; reproduction numbers continue to hover just above 1 (unchanged), and our models now project slow declines in case transmission in Staten Island, Manhattan and the Bronx. We forecast that cases will grow slightly in Queens and Brooklyn in the coming weeks before they reach their spring peak. Projected case numbers in bordering New York and Northern New Jersey counties appear to have plateaued.
- Reproduction numbers and test positivity rates have increased in most Pennsylvania counties to a similar magnitude that areas of Michigan began experiencing a few weeks ago. This has been accompanied by some modest growth in hospitalizations. Our models project continued growth in case incidence in the coming weeks across the state.
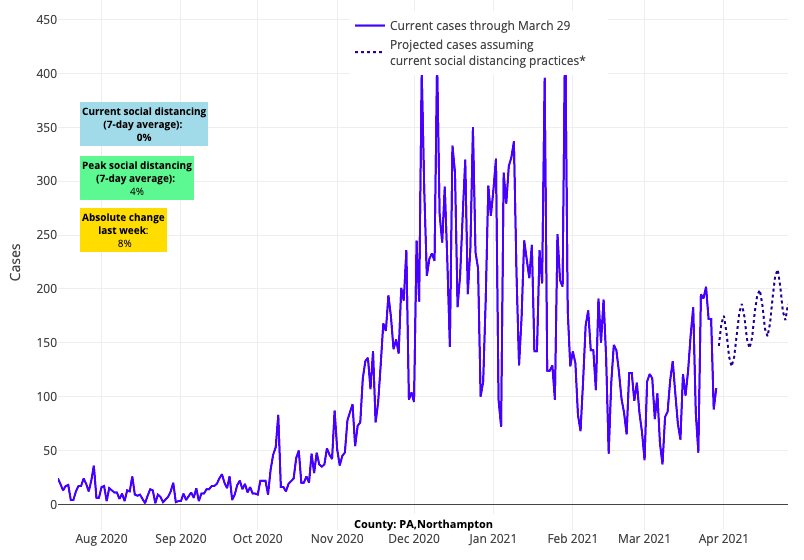
Above are the projections for Northampton County in Pennsylvania.
- In Florida, there are signs of stabilization with plateauing emergency department visits and hospitalizations. We continue to project flat case incidence over the next four weeks along Florida’s southeast coast. The Orlando and Tampa Bay/St. Petersburg regions, however, are demonstrating more accelerated community transmission; we forecast case incidence to rise in the coming weeks in these areas.
With just one day left in March, many counties throughout the country—particularly those in the north—continue to experience persistent or increased positivity and transmission rates. While Michigan may be reaching its spring peak, we are now concerned about a wider region including Ohio, Indiana, Illinois and Pennsylvania. (Fortunately, the current pace of disease spread and hospitalizations in these states is nowhere near what we observed this winter.) Even the Pacific Northwest, which has had some of the lowest case numbers throughout the pandemic, is seeing rising transmission and emergency department visits, particularly around Seattle.
As we have mentioned in prior weeks’ blog posts, there are multiple explanations for the trends we are seeing in this phase of the pandemic. One important factor is that Americans are on the move again, particularly this holiday week, which could increase transmission rates even more.
While increasing COVID-19 transmission across the country is certainly cause for concern, there are subtle indications that the severity of this resurgence, as measured by hospitalizations and deaths, will not be the same as we experienced last fall and winter, including:
- We are seeing reproduction numbers and case incidence begin to peak in the major cities of Michigan, which has been front and center for this current resurgence. The rate of growth in emergency department visits and hospitalizations is also beginning to slow and remains below 50% of the peaks we saw this winter.
- A key distinguishing feature of this phase of the pandemic continues to be the decoupling of community case incidence and hospitalizations. For example, although case incidence has remained quite high in the New York City boroughs and surrounding counties over the past several weeks, the growth in COVID-19 hospitalizations has been small. Similar trends, accompanied by improving test positivity, can now be seen in the Washington, D.C. metro area.
- Warming temperatures and longer days, which welcome more people outside where it is harder for COVID-19 to spread and may also reduce transmissibility, lend some confidence that states that see similar resurgence to that of Michigan’s may not eclipse, or even match, the peak that Michigan’s residents experience this spring. We see sustained improvements in much of the South, including in Florida and Texas, where spring weather has fully arrived. We hope this portends similar improvements in the north as residents there build immunity due to vaccinations, so that the region may eventually also reach a tipping point where the combination of spring weather and population immunity—particularly in older individuals—leads to a wider gap between community case incidence and hospitalizations.
- As vaccination rates increase across younger age groups, we suspect that hospitalizations will continue to abate, as will deaths. One needs to look no further than New York State over the month of March to see how vaccination is increasingly providing protection to older groups of individuals. Hospitalizations are down nearly 30% among individuals aged 70 and older and are flat among those between 60-70 years of age. For all other adult age groups, the rate of growth in hospitalizations is up 15-20%. The quicker we can get younger individuals vaccinated, the quicker we should see hospitalization rates decline across the country. Regions that experience similar resurgence to that of Michigan should benefit from rising vaccination rates, so long as they have steadily increased inventory and delivery to their residents. Those areas fraught with delayed delivery of vaccines to residents, particularly around densely crowded metropolitan areas, will be at greater risk for rising hospitalizations.
The picture that emerges from the data this week is one that reflects a younger population of children and working-age adults disproportionately represented in the growing case incidence throughout much of the country. Sadly, some unvaccinated working-age adults who get COVID-19 during this period will likely experience severe or even fatal disease. Some will be parents and grandparents, eager to gather and travel, but who have not yet been offered or who have declined vaccination. This is why the individual commitments each person makes to continue protecting one another, through masking in public locations and keeping gatherings small, is so important right now—even more so than any public restrictions. Those choices can ensure that as few families suffer the tragedies of this past year before vaccinations ultimately help us reach the tipping point we have all been yearning for.
