COVID-19 Outlook: Optimizing Pediatric Vaccination for COVID-19 & Influenza as Winter Approaches

Most children across the United States have returned to schools and early childhood education centers over the last few months. Their return followed a summer where COVID-19 transmission persisted in all areas of the country in both adults and children. This persistence should not come as a surprise as we anticipate COVID-19 infections will continue for many years. But as we transition out of the pandemic state(link is external) experienced over the past few years, we must shift to anticipate and prepare for the impact of COVID-19 illness during annual winter viral respiratory seasons.
In this update, we characterize the status of the upcoming fall/winter resurgence of COVID-19 as well as other respiratory viruses. We’ll focus particularly on the early seasonal impact on younger children, who lag considerably behind other age groups in their receipt of the primary COVID-19 vaccination series. We’ll also examine the current burden of COVID-19 and other respiratory viruses in children relative to prior years. The data reveal that the coexistence of these viruses is already posing a significant strain on hospital capacity for many pediatric health care systems.
Interpreting Current Trends Within the Context of Past Years
Following the omicron wave in the winter of 2021-22, COVID-19 infections increased in both vaccinated and unvaccinated individuals of all ages. Omicron’s transmissibility was partially driven by its ability to evade vaccine-induced immunity. As the numbers of vaccinated individuals infected by omicron grew, many erroneously believed that the vaccine was no longer effective. However, as we have noted in the past, the primary benefit of vaccination is protection against severe COVID-19 illness. As such, monitoring data on COVID-19 hospitalizations, as opposed to total case numbers, is now a more appropriate way of tracking the burden of COVID-19 illness at a population level.
Fortunately, adult hospitals experienced a 50% reduction in their average census this past summer, as compared to the summer of 2021, with declines continuing in late August and into September. However, while the number of pediatric admissions was also down across the last two summers, this decrease was less pronounced (down 20% from last summer) than the adult decline. It’s likely there were two factors contributing to the differing rates of decline between adult and pediatric hospitalizations. First, there were fewer overall pediatric hospitalizations to start and thus less potential for rapid declines. Second, there was less vaccine coverage for children, especially for those in younger age groups where COVID-19 vaccines were not approved until late in June 2022; thus, fewer children had vaccine-induced protection from COVID-related hospitalizations.
Even as national adult and pediatric hospital census reached a seasonal low this month, there is growing evidence of a winter resurgence of COVID-19. Declining hospital admissions and census nationally over the last few weeks has largely been the result of improvements in the South and West, particularly in larger states like Florida, Texas and California. Improvements in these regions may distract from an evolving resurgence in colder areas across the northern corridor of the country. For example, New England has been experiencing rising hospital admissions and emergency department visits for several weeks (see figure below), and there is growing evidence that a resurgence is beginning across the upper Midwest, Mountain West and Appalachian regions. Our team anticipates that national COVID-19 hospital census will begin growing again in the next couple of weeks as winter COVID-19 illness continues to expand across the country.
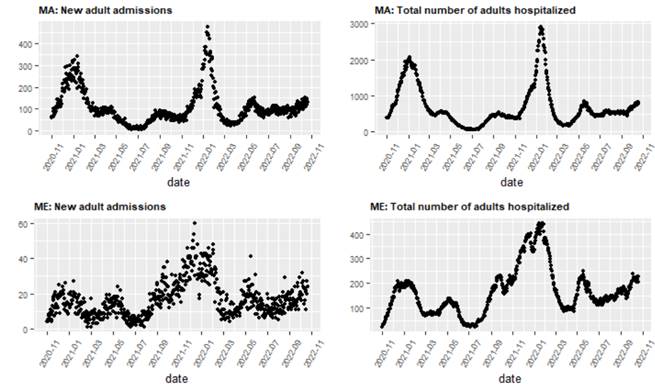
New adult admissions and total number of adults hospitalized in Massachusetts and Maine, 2020-2022
As this winter resurgence begins to take shape, our team examined recent regional and local trends in pediatric COVID-19 hospitalizations in the context of vaccination rates to gain insights on what we might anticipate in the coming weeks to months. This summer, more than half of all pediatric hospitalizations across the country were concentrated in the South, where primary vaccination rates in children are considerably lower than other areas of the country. Assessment of our own hospitalization data at Children’s Hospital of Philadelphia (CHOP) suggests a potential association between under-vaccination of children against COVID-19 and COVID-19-associated hospitalization. This is most apparent in children under 5 years of age, where primary series COVID-19 vaccination rates remain below 10% in our region (compared to 45% in children 5-11 years old and 60% in children 12-18 years old).
Earlier in the pandemic, children under age 5 comprised one-third of all our hospitalizations; they now comprise nearly two-thirds of our hospitalizations. The graph below shows the number of COVID-19-associated inpatient admissions our health system has had throughout the pandemic by age group. This figure identifies a subset of “likely COVID disease” from amongst all COVID-19-identified hospitalizations by prioritizing only those hospitalizations in which COVID-19 was listed as the primary diagnosis or when a COVID-positive diagnosis occurred during a hospitalization for an influenza-like illness. We remove hospitalizations in which children were admitted for other reasons (e.g., behavioral health or an exacerbation of a chronic illness), but were found to be incidentally COVID-positive during their hospital stay. Considering just the “likely COVID disease” hospitalizations, one can see that the number of children under 5 years old hospitalized for COVID-19 between March and early September 2022 remained consistently high well past the 2021-2022 winter season. This occurred even as admissions among older children largely declined and remained low.
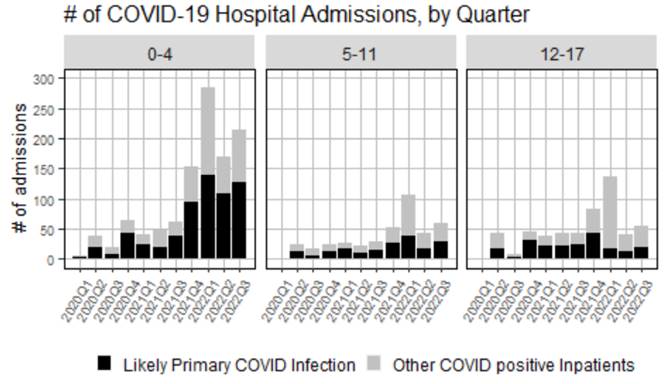
Number of COVID-19 hospital admissions by age group, 2020-2022
Importantly, we also need to recognize the presence of other circulating respiratory viruses leading to pediatric hospitalizations(link is external) as winter approaches. For the last few years, mitigation strategies like masking not only helped to reduce COVID-19 hospital admissions, but also limited illness from other respiratory pathogens like RSV or influenza. However, these other pathogens are now returning, and much earlier than their typical seasonality. Pediatric hospitals like ours are experiencing a substantial rise in RSV infections among their hospitalized patients, and are now beginning to detect the onset of a resurgence of influenza admissions, which typically arrive later in the winter.
Collectively, hospitalizations from COVID-19, influenza, RSV, and other respiratory pathogens are likely to continue to climb and remain high well into the new year. Hospital administrators are already noting the burden that these admissions are having on their inpatient capacity and are planning for even higher increases, further emphasizing the need for vaccinating all eligible children against COVID-19 and influenza to reduce hospitalizations for the coming winter.
Educating Families on the Importance of Primary COVID-19 Vaccination in Young Children
Even as our public health colleagues introduce new boosters to prevent severe COVID-19 infections in previously vaccinated adults in advance of this winter, it is important to highlight that among our pediatric colleagues, the primary COVID-19 vaccination series for young children remains a higher priority. Many children remain unvaccinated or incompletely vaccinated despite U.S. Food and Drug Administration authorization for children down to age 6 months to receive the vaccine since the end of June 2022.
Though data supports the safety and effectiveness of COVID-19 vaccines in all pediatric age groups, caregivers continue to be hesitant to vaccinate their children. Recently, Kaiser Family Foundation(link is external) surveyed families about their willingness to get their children vaccinated. The results were sobering and included:
- More than 4 in 10 parents of children ages 6 months through 4 years say they will “definitely not” get their child vaccinated against COVID-19.
- Unvaccinated parents are particularly likely (64%) to say they will “definitely not” vaccinate their youngest children.
- When asked in their own words the main reason why they will not vaccinate their eligible child under 5 “right away,” parents cite concerns about the newness of the vaccine and not enough testing or research, concerns over side effects, and worries over the overall safety of the vaccines.
- Most parents of children under 5 years who are now eligible for the vaccine say they have not spoken to their pediatricians or other health care providers about the vaccine for their child (70%). Among parents considering vaccination for their child, most (70%) say they will wait until their child’s regular check-up to discuss getting them vaccinated.
As winter approaches, it is becoming increasingly likely that children, particularly those who are younger, will be exposed to rising risk of infection and hospitalization due to COVID-19 at the same time they will face a higher risk from influenza, RSV and other viral respiratory infections. This additive risk may make this winter a difficult one in many households, but families still have the opportunity to reduce the risk of severe illness for their children by reaching out to their pediatricians to learn more about these vaccines and to schedule appointments for vaccination.
Recognizing an urgent need for a comprehensive education strategy to better inform pediatric primary care clinicians, school and daycare leadership, and caregivers about navigating this winter’s “sick season,” our colleagues at CHOP have produced very useful educational materials to guide families over the holiday season. This type of educational strategy can be strengthened through a collaborative public health effort and amplified by well-informed media outlets. Simplified messaging must also be accompanied by efforts to improve access to seasonal vaccinations, beyond simply depending on primary care locations to meet this need.
If we can highlight the unique impacts we are seeing in children, and if we can urgently address issues of access to vaccination outside of periodic check-ups, there is potential to optimize vaccine coverage in the coming weeks with the intended goal of reducing the burden of severe viral illness over the 2022-23 winter season.
Jeffrey Gerber, MD, PhD, is associate chief clinical research officer of Children’s Hospital of Philadelphia's (CHOP) Research Institute and co-author of PolicyLab and CHOP's Guidance for Updated COVID-19 School Mitigation Plans for Academic Year 2022-23.
